The bombs that made Boston look like a combat zone have also brought battlefield medicine to their civilian victims. A decade of wars in Iraq and Afghanistan has sharpened skills and scalpels, leading to dramatic advances that are now being used to treat the 13 amputees and nearly a dozen other patients still fighting to keep damaged limbs.
“The only field or occupation that benefits from war is medicine,” said Dr. David Cifu, rehabilitation medicine chief at the Veterans Health Administration.
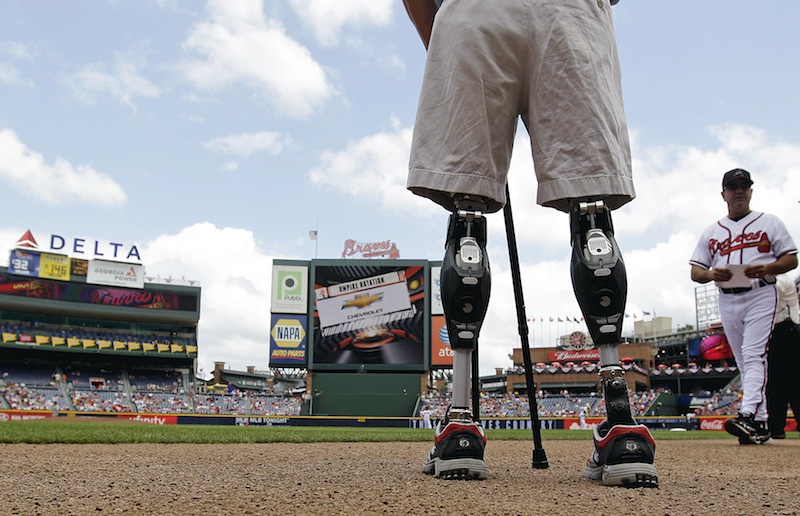
Nearly 2,000 American troops have lost a leg, arm, foot or hand in Iraq or Afghanistan, and their sacrifices have led to advances in the immediate and long-term care of survivors, as well in the quality of prosthetics that are now so good that surgeons often chose them over trying to save a badly mangled leg.
Tourniquets, shunned during the Vietnam War, made a comeback in Iraq as medical personnel learned to use them properly and studies proved that they saved lives. In Boston, as on the battlefield, they did just that by preventing people from bleeding to death.
Military doctors learned and passed on to their civilian counterparts a surgical strategy of a minimal initial operation to stabilize the patient, followed by more definitive ones days later, an approach that experience showed offered the best chance to preserve tissue from large and complex leg wounds.
At the same time, wartime demand for prosthetics has led to new innovations such as sophisticated computerized knees that work better than a badly damaged leg ever would again.
“This is a clear case where all of the expertise that was gained by prosthetic manufacturers was gained from the wars. It’s astonishing how well they function and the things people can do with these prostheses,” said Dr. Michael Yaffe, a trauma surgeon at Beth Israel Deaconess Medical Center in Boston.
The hospital has performed amputations on three blast victims so far. A few other patients there may yet need them. Yaffe is a lieutenant colonel in the Army Reserves, and many other doctors treating Boston blast victims also have had military training.
Besides the three at Beth Israel, five patients who have lost a total of eight limbs are at Boston Medical Center; four who each lost a leg are at Massachusetts General and one who lost one limb is at Brigham and Women’s Hospital.
The military partnered with the American Academy of Orthopaedic Surgeons to train doctors throughout the United States on advances learned from the wars, said Dr. Kevin Kirk, an Army lieutenant colonel who is chief orthopedic surgeon at San Antonio Military Medical Center.
Help, too, has come from Israel, which for decades has dealt with the aftermath of Palestinian bombs, like the ones in Boston, often laden with nails, ball bearings and other metals.
“Unfortunately, we have great expertise,” said Dr. Pinchas Halpern, director of emergency medicine at Tel Aviv’s Sourasky Medical Center.
Halpern, who gave lectures in 2005 at Brigham and Women’s Hospital and Massachusetts General about responding to attacks, has been in email contact with doctors in Boston this week.
Among the topics he covered in his lectures were how to coordinate ambulances to distribute the wounded to area hospitals according to their type of injury, performing more CT scans than usual to locate deep shrapnel wounds, and ways to identify and classify wounds. Dr. Paul Biddinger of Mass General’s emergency department said the hospital took much of Halpern’s advice.
“We improved our plans for triage, site security, reassessment and inter-specialty coordination” following Halpern’s visit, Biddinger said.
Blast victims can be challenging to treat because they typically have multiple complex physical injuries that may include loss of limbs, fractures, brain damage, and vision and hearing impairment, said Dr. Paul Pasquina, chairman of physical medicine and rehabilitation at the Uniformed Services University and Walter Reed National Military Medical Center.
“It’s very important that during their acute medical and surgical care that rehabilitation is applied early on, to get them up as soon as possible” to reduce risks from being immobile, including blood clots, deconditioned muscles and other problems that will make recovery more difficult,” he said.
A multidisciplinary approach that involves everyone from plastic and orthopedic surgeons to therapists is important, said Dr. James Ficke, chairman of the department of orthopedics and rehabilitation at San Antonio Military Medical Center. He also advises the U.S. Army Surgeon General on orthopedics.
“The lessons we’ve learned are early surgery, multiple surgeries and getting them back to skilled facilities in a fairly fast fashion,” he said.
“As a doctor, one of the lessons I learned most dramatically is I don’t have any preconceptions of what they can or can’t do as a patient. There was a patient who lost his leg completely and had no hip joint and recently did a marathon in Austin in 4:33.”
For some, that may mean a prosthetic leg. John Fergason, chief prosthetist at Center for the Intrepid, the outpatient rehab center at the San Antonio medical center.
Brooke Army Medical Center, said there have been many advances, including computerized knees that allow amputees with above-the-knee amputations to walk down steep ramps, to walk up steps and go from a walk to a run.
After every war, “you see a tremendous spike in prosthetic innovation,” largely because of increased research money, said Hugh Herr, a prosthetic expert at MIT and a double-amputee himself. Federal funds let his MIT lab do basic research on a bionic foot-ankle-calf system, and he founded a company that has commercialized that device.
If Boston victims are generally healthy and motivated, and their legs are amputated below the knees, or perhaps even above the knees, “it’s possible they could run the marathon a year from now,” he said. “It would take a lot of effort, but it’s indeed possible with today’s technology.”
One amputee’s story is encouraging.
Dan Berschinski, 28, used to run marathons but now works with the Amputee Coalition, an advocacy and support organization based in suburban Washington, D.C. He was an infantry officer in Afghanistan when he stepped on an IED in August 2009. The blast blew off his entire right leg and most of his left leg. After treatment in the field and in Germany, he was sent to Walter Reed.
His biggest initial challenge was intense pain, treated with narcotic painkillers, and phantom leg and foot pain. Doctors used to consider phantom pain a psychological problem but now consider it real, physical pain. Treatment includes nerve blockers.
“If they hit you really hard with a combination of narcotics and nerve drugs, people have a lower incidence of phantom pain the rest of their life,” Berschinski said.
Recovery and rehab took about three years, including 10 months of daily physical therapy to strengthen his arms and core — muscle power he’d need to learn to walk on prosthetics.
The bionic legs he uses cost $60,000 a piece, are hydraulically operated and equipped with microchips and a gyroscope that sense when to relax and stiffen to help him walk. Walter Reed was involved in developing the legs, said Zach Harvey, former prosthetics chief at Walter Reed.
Berschinski used to run marathons but now can go only about half a mile. He competes in triathlons — swimming, biking with his arms, and racing in a wheelchair, and sometimes plays wheelchair basketball.
“I’m very happy with my progress,” he said.
Send questions/comments to the editors.




Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.