CHICAGO — November was Lung Cancer Awareness Month, but you’d never know it. Consumers aren’t bombarded by products in blue, the color designated by some to raise the profile of the disease. No NFL players or coaches wore blue-ribboned apparel, despite donning pink just a month earlier for breast cancer.
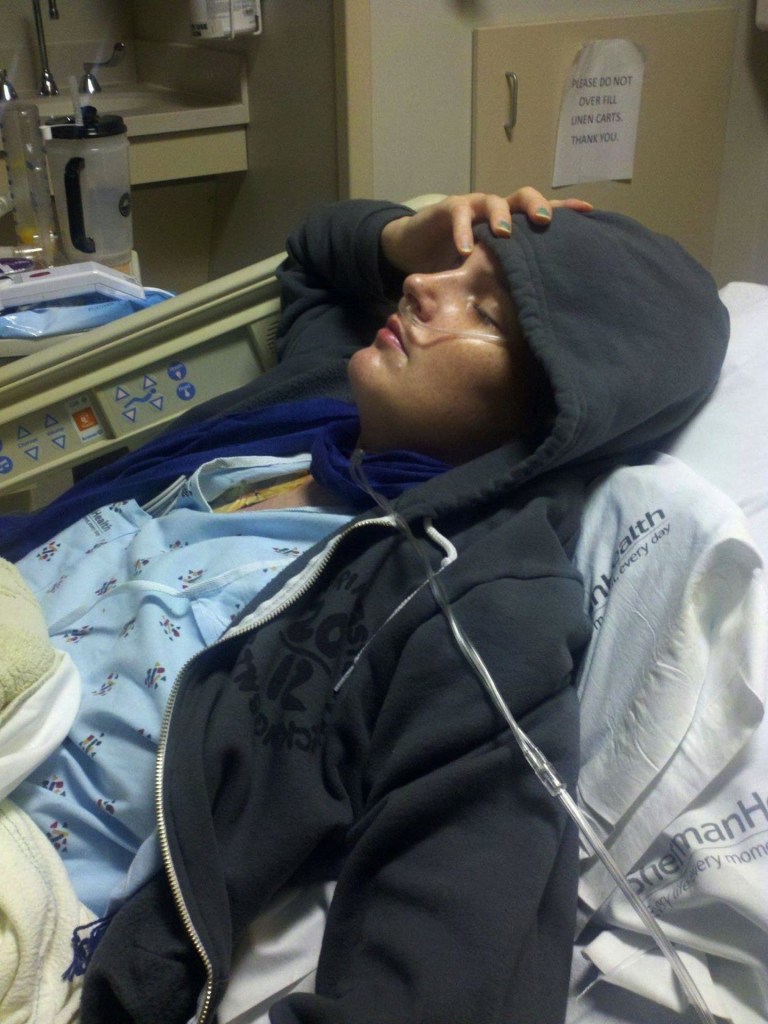
“It just doesn’t seem fair,” said Meghan O’Brien, 31, a nonsmoker diagnosed with stage 4 of the disease last year. There is no stage 5.
The lack of buzz is especially perplexing because lung cancer is the leading cause of cancer death in the United States, claiming more lives than breast, prostate, colon and pancreatic cancers combined. The five-year survival rate is just 16 percent _ a statistic that has barely budged since 1975, according to the American Cancer Society.
But lung cancer is seen as a tobacco-related illness that patients somehow bring upon themselves.
About 10 to 15 percent of the roughly 228,000 people diagnosed with the disease each year were never smokers, according to the LUNGevity Foundation, a Chicago-based support organization.
Stigma negatively affects everything from emotional support to the anemic November awareness campaign. Even in obituaries, family members feel compelled to include the “nonsmoker” status, lest the deceased be unfairly judged.
DISPARITY IN FUNDING
However, nowhere is the disparity felt more acutely than in funding research. The National Cancer Institute estimates that $17,835 is spent per breast cancer death versus $1,378 for lung cancer, even though lung cancer accounts for almost 23,000 deaths annually among nonsmokers.
“If we don’t start paying attention and changing attitudes, we will have a losing battle ahead of us,” said Dr. Ravi Salgia, O’Brien’s oncologist at University of Chicago Medicine.
Not that it’s easy to build awareness. Forget the pink marketing blitz; just try to find a ribbon for lung cancer. There’s even dispute over the appropriate color, according to Andrea Ferris, president and chair of the LUNGevity Foundation, who says it’s blue. Others say it’s clear or pearl.
“In every other disease, the first question people ask is, ‘How can I help?’ But with lung cancer, there’s no empathy. It’s always, ‘Did you smoke?’ After a while, it’s just easier not to say anything,” Ferris said.
In O’Brien’s case, doctors pinpointed a rare genetic mutation, called ALK, created when two normal genes fuse together to form a new, cancer-causing one.
The University of Chicago is one of the nation’s major treatment centers because of a clinical trial for crizotinib, part of a new arsenal of drugs designed to help patients by blocking ALK. This pharmaceutical “Hail Mary” helped contain O’Brien’s cancer for a while, but now it has come roaring back, invading her lungs and brain. Two months ago, a scan revealed a liver studded with tumors.
‘BLAME AND SHAME’
The Huntley woman is now in another early stage clinical trial and channeling her waning energy into chipping away at the “blame and shame” that has impeded progress. She also started a blog to chronicle her lung cancer journey.
“I try not to get too mad when people ask if I smoked,” she said. “Instead, I try to turn it into an opportunity to talk about it … to educate. I guess that’s the teacher in me.”
Even so, O’Brien immediately recited her virtuous health habits: Physical education teacher. Avid tennis player. An “almost vegetarian” who hasn’t rolled through a fast-food window since age 13. No cigarettes, ever.
At first she had experienced back pain, which she attributed to muscle strain, a logical explanation for someone so active. But in May 2012 it became excruciating. She went ahead with X-rays, paying the $600 tab herself because, as a teacher’s aide at New Trier High School, she didn’t have health insurance. The results were inconclusive.
By the end of summer she had landed a full-time job teaching physical education at Kenwood Academy High School in Hyde Park, allowing her to move out of her parents’ home and into her own apartment in Bridgeport.
“I was so excited because it had a big yard for my dog,” she said. “Also, I thought I might be able to get a job working for the White Sox in the summer, combining my two loves of education and sports.”
UNEXPECTED DIAGNOSIS
However, just as her “grown-up life” was taking off, it splintered apart.
She received varying diagnoses, including scoliosis, sinus infection and pneumonia. On Sept. 1, the first day of her new job, she went to her neighborhood clinic. The physician took one look at her test results and sent her to University of Illinois at Chicago’s emergency room. Six hours later, a nurse told her to call her parents.
Even after being admitted to the oncology floor, cancer didn’t enter her mind. “I thought maybe this was the only place where they had an open bed … or it was pneumonia or tuberculosis, and this was the only room where I could be quarantined.”
But two weeks later, a doctor confirmed the worst: stage 4 non-small cell lung cancer, already assaulting other organs. All she remembers is her father reaching out to steady himself on a nearby radiator.
O’Brien spent most of the next four months in the hospital. Before she could start therapy, she needed emergency spinal surgery to remove the malignant tumors wrapped tenaciously around her spinal cord.
UNFULFILLED DREAMS
After discharge, O’Brien moved back to Huntley so her parents could help with her care. After almost three years of trying to obtain a full-time teaching job, her tenure at Kenwood had lasted about a month.
O’Brien’s eyes glistened with tears as she ticked off her unfulfilled dreams – having a profession, getting married, having kids, buying a home.
“When I was first diagnosed, I asked about freezing my eggs,” she said. “They basically told me that there was no point because I wouldn’t live long enough … to get the procedure done.”
Besides, she said, dating isn’t really on her radar now. Treatment caused her to lose her hair, while steroids added 50 pounds.
The ultimate indignity, she said, “is when people ask, ‘Are you sure you never smoked?’ As if I forgot.”
Not that anyone deserves the deadly diagnosis. It wasn’t so long ago that the military dispensed cigarettes to soldiers, and many lung cancer patients kicked the smoking habit decades ago, she said. “But it doesn’t matter. … People still think it’s your fault.”
CONDEMNATION
As a leading clinician-scientist in lung cancer, Salgia has seen the condemnation firsthand. He also can see a more hopeful landscape, especially with the advent of new genetic therapies that may replace traditional chemotherapy and radiation. “The era of precision oncology has arrived,” he said.
Better screening and biomarker tests also are on the horizon, identifying people earlier and improving outcomes. But none of it may happen without removing significant political, social and financial barriers.
“Look at what we did with AIDS in the 1990s,” Salgia said. “Our job is not to judge … but to ask, ‘How do we prevent this disease? How do we cure it? How do we face this together?’ ”
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.