A special committee led in part by U.S. Sen. Susan Collins, R-Maine, is putting a federal focus on the rising costs and other challenges of providing long-term care for a growing number of older Americans.
Long-term care in an assisted-living facility or nursing home costs $42,000 to $90,000 per year in the United States, and few Americans are prepared to foot the bill, experts told the U.S. Senate Special Committee on Aging last week.
The annual tab for long-term care in the United States was more than $200 billion in 2011, and the cost is expected to skyrocket because the number of Americans who need long-term care now – 12 million – is on track to more than double by 2050.
Meanwhile, unpaid caregivers, found in nearly one-third of U.S. households, are providing an additional $400 billion in uncompensated care annually that puts untold strain on families, employers and communities.
“So many of us are living longer, more and more Americans need long-term care, and that need is only going to soar,” said Collins, who is the ranking Republican member of the committee, which is chaired by Sen. Bill Nelson, D-Fla.
The 19-member committee on aging held its first hearing on long-term care concerns on Wednesday, focusing on a recent report from the Commission on Long-Term Care, which was created in January when the American Taxpayer Relief Act of 2012 was signed into law.
Collins said the committee on aging, on which she has served since she first went to Washington in 1997, will continue studying several troubling aspects of long-term care in the coming year and hopes to develop legislation that will bring some solutions.
“We’re putting a spotlight on an issue that is beyond partisanship,” Collins said. “It needs to be confronted with a multipronged, nonpartisan approach.”
It’s the first time a federal legislative committee has homed in on long-term care problems, which are growing along with the population of Americans age 65 and older.
The number of seniors is expected to more than double, from 40.2 million in 2010 to 88.5 million in 2050, reflecting a global aging trend, according to the U.S. Administration on Aging.
Long-term care challenges are especially acute in Maine, which is the oldest state based on median age (43.5 years) and the second-oldest based on proportion of people age 65 and older (17 percent), according to the U.S. Census. Florida is No. 1 with 18.2 percent. Maine also has the highest proportion of baby boomers – 29 percent of its 1.3 million residents were born between 1946 and 1964.
The Portland Press Herald/Maine Sunday Telegram is examining various impacts of Maine’s rapidly aging population in a special investigative series, “The challenge of our age,” which shows that the state isn’t taking good care of its seniors now and isn’t prepared for what’s coming down the road.
Collins said the 150-seat committee room was uncommonly packed on Wednesday and that several people remarked that they were glad long-term care issues were finally being addressed in Congress.
Lori Parham, director of AARP Maine, shares their enthusiasm.
“Issues related to long-term care are often viewed as state issues,” Parham said. “It’s great to see recognition at the national level of the challenge we face in this area.”
Commission members and others testified that, in addition to rising costs, the United States faces a shortage of workers to meet the growing demand for community and in-home care as the preferred long-term care options.
The commission recommended improving training, pay and advancement opportunities for long-term care workers, according to the written record of testimony by Dr. Bruce Chernof, commission chairman. He heads The SCAN Foundation, an organization in Long Beach, Calif., that promotes aging with dignity and independence.
The commission called for a sustainable balance of public and private financing for long-term care, Chernof testified, including a rebalancing of Medicare funding priorities to promote community and in-home care as less costly than nursing homes.
The commission also recommended adopting tax incentives that would encourage people to start saving early for long-term care, such as dedicated tax-exempt IRAs and annuities or tax-deductible insurance premiums.
Currently, about 7 million Americans have long-term care insurance – about 12 percent of the population age 65 and older, said Anne Tumlinson, senior vice president of long-term care at Avalere Health, a health care consulting firm in Washington, D.C.
“The challenge lies chiefly in the question of persuading individuals to enroll in an insurance program that they do not know they need and won’t use for up to 30 or 40 years,” Tumlinson testified before the committee.
Collins said that in her experience, many people don’t realize that federally funded Medicare doesn’t pay for long-term care other than for rehabilitation after a hospital stay. When people run out of their own resources, they wind up on federally and state-funded Medicaid.
“Just as we plan for retirement, we need to be planning for long-term care,” Collins said.
Kelley Bouchard can be contacted at 791-6328 or at:
kbouchard@pressherald.com
Twitter: @KelleyBouchard
Send questions/comments to the editors.

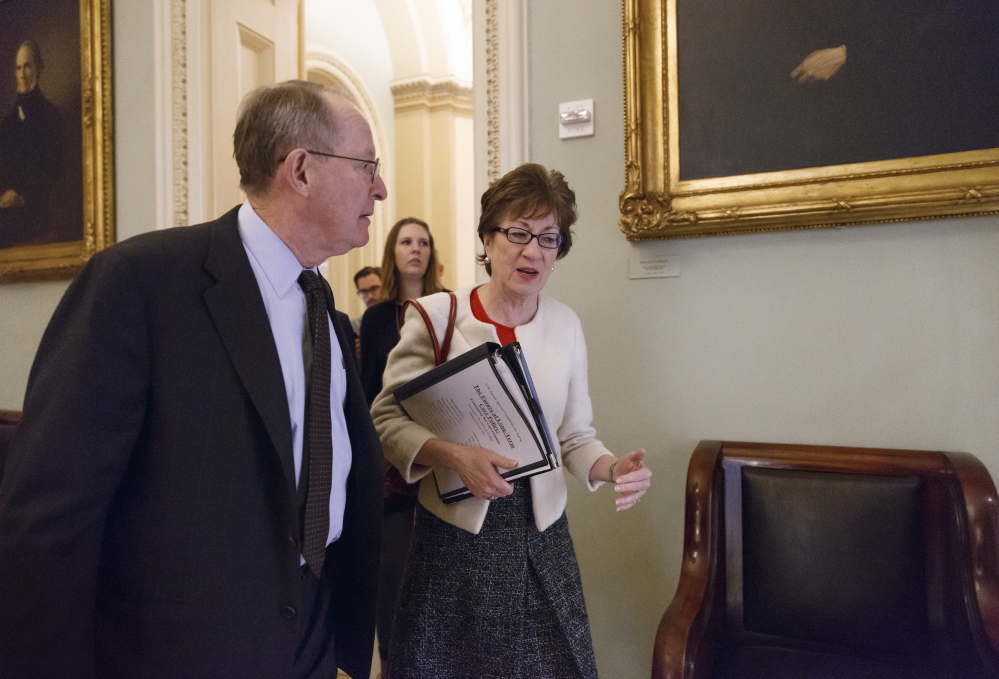

Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.