The state’s financial commitment to fighting the heroin and opiate epidemic has decreased during a time when drug overdose deaths have soared into unprecedented territory and as demand for treatment far outstrips available resources.
Maine spent 6.6 percent less, or about $4.5 million, on drug treatment and prevention overall from fiscal year 2014 to fiscal year 2015, according to information provided by the Department of Health and Human Services.
But DHHS Commissioner Mary Mayhew said the numbers provided by her office don’t include all spending and that the amount spent should not be the benchmark for success. She said efforts to combat the crisis have been made even if the results aren’t yet visible, and more is being done every day.
“Certainly, when it comes to substance abuse and when it comes to prioritizing spending, there are a host of spending priorities,” Mayhew said in an interview Friday. “Because it is multifaceted, we need to ask, how do we make sure we’re adequately funding law enforcement, prevention and treatment? We need to ask, what are the most effective ways?”
Much of that drop in spending was in MaineCare reimbursements, which makes sense because Maine no longer allows a category of clients – able-bodied adults without dependents – to access MaineCare. It was Gov. Paul LePage and Republican allies who pushed to cut access to some of the poorest Mainers, arguing that the program was becoming unsustainable.
Mayhew said the state has committed $20 million in funding to the uninsured, but providers have argued that money just isn’t reaching those who need it.
Other than MaineCare, the biggest expenditures come from a federal grant program administrated by the Substance Abuse and Mental Heath Services Administration. Maine received more than $2 million less for the current fiscal year under that program. Also, the state has been using more and more of its federal dollars for preventive programs, rather than treatment programs. Other states with similar populations, however, are doing the opposite.
The modest amount of emergency funding for treatment that the Legislature did approve this spring – billed by both Democrats and Republicans as only a first step – has yet to yield full impact.
‘WE HAVEN’T HAD MUCH ACTION YET’
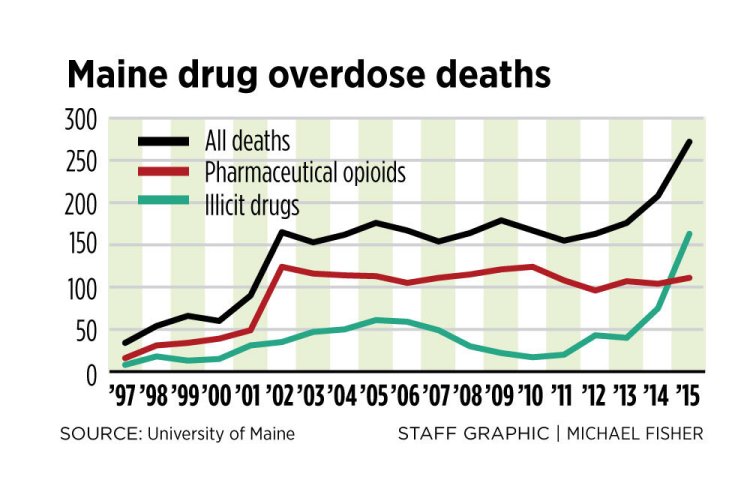
Meanwhile, there have been 189 overdose deaths in the first six months of 2016, far ahead of last year’s pace, and last year saw the highest number of overdose deaths ever recorded, at 272. The state could not provide updated treatment statistics last week but previous reports indicate that the number of people seeking treatment for heroin addiction alone rose from 1,110 in 2010 to more than 3,500 in 2014.
“I don’t think there is any question that we haven’t done enough,” said state Sen. Anne Haskell, D-Portland. “We can’t just throw money at a problem, but there are few solutions that don’t have a cost, so it’s nonsensical to think that we’re not going to have some investment.”
Sen. Eric Brakey, a Republican from Auburn who co-chairs the Health and Human Services Committee and is a firm proponent of limited government, agreed that more can and should be done to combat addiction.
“It’s easy to say yes to things that don’t cost taxpayers money, and when we talk about programs that do cost money, we should do a cost-benefit analysis,” he said. “But I would happily take dollars away from incarcerating people for drug offenses and put that toward treatment.”
Mayhew stressed it’s the Legislature that approves funding, but the LePage administration has not prioritized increased spending in treatment. Instead, he has focused more attention on beefing up law enforcement resources and attacking the supply of illegal drugs.
Mayhew said the amount of funding for treatment is not as important as how it’s being used. She said the state is committed to identifying best practices and supporting innovative programs, although she acknowledged that there are differing opinions about what constitutes effective treatment programs.
The feeling by some substance abuse providers is that the state simply isn’t moving as quickly as the crisis demands. They have been saying for years now that the state does not have nearly enough detox beds, residential inpatient beds or doctors able to administer medication-assisted treatment such as suboxone. Providers say they are frustrated at having to tell patients that they can’t provide help, knowing that some of them could end up dead without treatment.
Steve Cotreau, program manager at the Portland Recovery Community Center, a support group and resource for those trying to recover from addiction, said he has seen a surge in people seeking help. He said the center tries to connect people with treatment, but many times it’s “almost impossible” because of the lack of resources available in Maine.
“This is very disheartening,” Cotreau said. “There’s been a lot of talk, but talk doesn’t solve anything. We haven’t had much action yet to solve this problem.”
FOLLOWING THE MONEY ISN’T EASY
Tracking the amount of state money spent on the drug crisis is difficult, in part because the LePage administration has provided differing – and sometimes conflicting – numbers.
In early 2014, when the heroin/opiate crisis was taking hold but before it exploded, the state released information that indicated overall spending on substance abuse treatment dropped from about $47 million in 2010 to $43.7 million in 2011.
That $47 million still represented only 3.4 percent of the $1.4 billion total estimated cost of drug and alcohol abuse in Maine, including medical, criminal and incarceration costs.
Last year, the administration pointed out that the annual budget for the Office of Substance Abuse had increased from $18.6 million in fiscal year 2010 to $21.5 million in the 2015-16 fiscal year – an increase of 16.6 percent over a five-year period. What was left unsaid was that in 2012, the Office of Substance Abuse merged with the Office of Adult Mental Health Services.
During that same time last year, LePage said the state had “increased funding for addiction treatment from $7 million to $17 million since I’ve been governor,” beginning in 2011. The administration never explained the discrepancy in those numbers.
The governor said during a radio address that his Department of Health and Human Services had plenty of money available for drug treatment, even for those who are without Medicaid or private insurance.
That revelation came as a surprise to the substance abuse community.
Earlier this year, Mayhew also said that providers were not spending all their contracted money and were not supplying enough data about what methods were effective.
NO NEW FUNDING FOR MEDICATION-ASSISTED TREATMENT
DHHS funding data in June showed that between fiscal years 2012 and 2015, spending on addiction treatment dropped by more than $5 million overall, but by more than $7 million within MaineCare. That was $4.7 million less on counseling, $2 million less on medicated-assisted therapy and $2.6 million less on residential treatment.
Mayhew said the spending figures provided by her office this year were accurate but did not reflect all the state’s efforts. For instance, they didn’t include transportation costs for patients who need to travel for treatment, such as trips to methadone clinics. She also said it doesn’t include the administration’s commitment to supporting behavioral health homes, some of which house people battling substance abuse.
In January, after everyone in the Legislature seemed to agree that the drug crisis was dire and in need of emergency funding, lawmakers passed a bill that authorized $3.7 million in spending: $2.5 million for treatment and the rest to hire new drug enforcement agents. That money came from the state’s medical marijuana fund.
LePage’s focus on law enforcement so far has yielded a sharp increase in the number of drug trafficking arrests in the last few years. But overdose deaths are still skyrocketing, suggesting that the drugs are still getting into Maine.
About $1 million of the extra spending in the bill was to pay for a 10-bed detox facility in Bangor that has yet to open. The state has put the project out to bid twice and changed its mission from a traditional detox to a “social detox” that will not provide medication-assisted treatment. An additional $800,000 was set aside to increase access to residential treatment and outpatient services for the uninsured.
The remaining $600,000 or so was earmarked to establish more peer recovery centers in underserved parts of the state.
No new money has been put into medication-assisted treatment, which experts say is the best and most cost-effective way to treat people with opiate or heroin addiction.
Malory Shaughnessy, executive director of the Alliance for Addiction and Mental Health Services, Maine, said providers feel they are being asked to do more with less. She said the state has been doing more inspections and demanding more paperwork, which takes time away from providing care.
“Our providers already use evidence-based practices,” she said. “They are trying to meet the need coming through their doors.”
EXPANDING ACCESS TO TREATMENT
Over the last five years, the state has applied for and received more than $21 million in federal funding for prevention programs but only about $6 million during that period for treatment.
Meanwhile, other states with similar populations that are dealing with an opiate crisis, including Vermont, Idaho and West Virginia, have sought more federal funding for treatment, because that’s where demand is highest. Idaho, for instance, has spent $21.5 million of its federal dollars on treatment and about $7 million on prevention in the last five years. Vermont has split its federal funds pretty evenly since 2011-12, with $17 million going to prevention and $15 million to treatment.
When asked about Maine’s use of more federal SAMHSA funds for prevention over treatment, Mayhew said she would have to look into that further. But she did say that in the most recent budget, the state repurposed some prevention funding for treatment.
A state task force convened last year by LePage, following a particularly deadly stretch of overdoses, met for several months before producing a report outlining recommendations.
One of those recommendations, perhaps the one that would have the greatest and most immediate impact, is one that does not have support from the governor or the divided Legislature: expanding access to MaineCare, as allowed under the federal Affordable Care Act.
LePage and Republican allies in the Legislature have fought multiple attempts at expanding MaineCare, saying it will be far too costly. Under the ACA, expansion would be paid for almost entirely with federal dollars for the first three years, but LePage and others say the government may not be able to keep that promise and worry about what happens after those first three years.
Sen. Haskell acknowledges that expanding Medicaid is a nonstarter with the governor and most Republicans. But she asked what the alternative would be.
“What we’ve done has been Band-Aids,” she said. “We’ve done some good work but it’s not enough. We’re nowhere.”
SOME COMMUNITIES AREN’T WAITING FOR HELP
LePage has supported expansion of suboxone and has pushed to adopt some of the most stringent prescription monitoring requirements for doctors, in an effort to keep prescription opiates to a minimum. But the administration also has pushed to change the rules for methadone clinics, which the clinics say could hamper their ability to treat as many patients as needed. Already, many methadone clinics have a waiting list and limits on the number of patients.
Mayhew said her department also is exploring pilot programs to make another treatment drug, Vivitrol, available.
Some communities already have begun to address the problem without waiting for more state funding.
Operation Hope in Scarborough is modeled on a program launched last year in Massachusetts that uses the police department as a conduit to treatment.
Meanwhile, a $1 million plan by a new group – the Greater Portland Addiction Collaborative – aims to use limited resources to expand programs that are already in place rather than attempt to create new programs. The collaborative, which formed in December, includes a group of nonprofit organizations, the city of Portland, Mercy Hospital and substance abuse treatment advocates.
Correction: An earlier version of this story misspelled Malory Shaughnessy’s name and misidentified her organization.
Send questions/comments to the editors.





Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.