AUGUSTA – Maine leads the nation in drug takeback efforts, in which citizens voluntarily return unused pharmaceuticals to keep them out of the environment and the hands of those who would sell or abuse them. Year after year, Mainers have handed in tens of thousands of pounds of drugs during federally sponsored national takeback days, more per capita than any other state.
But expected changes in federal and state policies could weaken some of the programs’ benefits, both in terms of environmental protection and in driving down health care costs. The state is seeking to change how collected drugs are disposed of, while proposed changes on the federal level would outlaw efforts to tabulate what drugs are being wasted.
The U.S. Drug Enforcement Agency has proposed rule changes for drug takeback programs that forbid authorities from gathering data on what drugs are being returned and in what quantities. Such data has been used to reduce the cost of MaineCare — the state’s Medicaid program — by imposing 15-day limits on the initial prescriptions of often-wasted drugs, many of which are opiates.
“If we see a certain drug that is being wasted a lot, we can come up with programs that might reduce that, for instance by changing prescribing behavior,” said Rodney Larson, founding dean of the Husson University School of Pharmacy, who has been involved in the tabulating of returned drugs by the University of Maine Center on Aging. “This is valuable information, and DEA’s new regulations forbid it from happening in the future.”
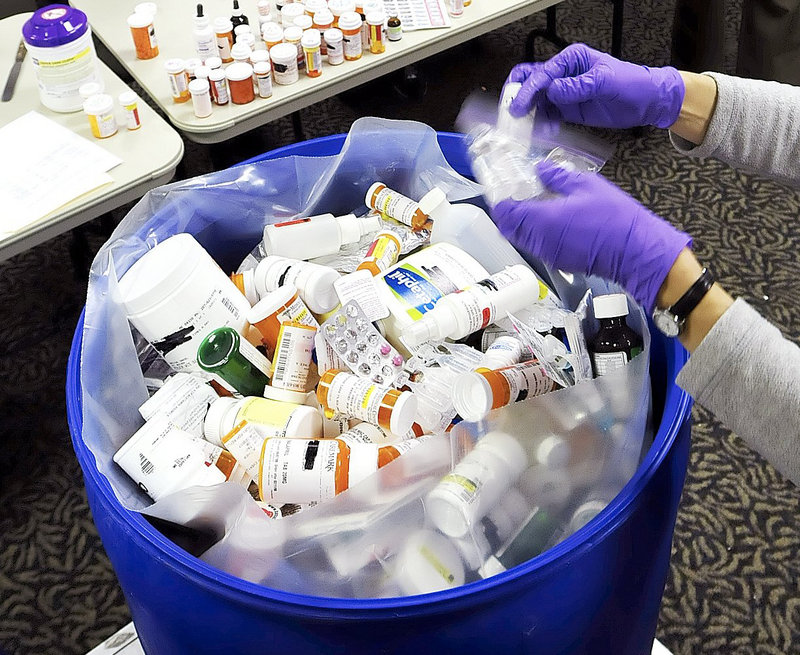
Researchers — many of them pharmacy students — have counted drugs returned to collection boxes at Maine pharmacies and by a now-defunct mailback program while under close supervision by law enforcement. But the proposed federal rules say collected drugs “may not be individually handled, counted, inventoried, or otherwise discerned.”
The DEA says it considered allowing authorized people to collect data but that such efforts “would require individualized identification of the contents, increase the number of hands through which controlled substances pass and … greatly increase the risk of diversion” to illegal users. It concluded that the risks “outweigh the potential benefits.”
Asked whether the DEA had considered the potential cost savings to state Medicaid programs, DEA spokeswoman Barbara Carreno declined to comment, citing the provisional nature of the rule.
The proposed rules are undergoing a 60-day public comment period that ends Feb. 19.
Sen. Susan Collins — who spearheaded key 2010 federal law supporting drug takeback programs — expressed concern over the proposed measure on learning of it from a reporter.
“It is important that these drugs are inventoried, in a way that respects the privacy of patients, before they are destroyed,” Collins, R-Maine, said in a written statement. “This helps determine exactly what drugs are being prescribed and purchased, but are going to waste … (which) can lead to better prescribing practices, improved patient education, and lower health care costs.”
“I intend to ask the DEA to further explain why its proposed rule would prohibit the gathering of this information,” Collins said.
Nationally, an estimated 40 percent of drugs prescribed outside of hospitals go unused, creating a health and environmental hazard. Flushed down the toilet or discarded in landfills, their contents can contaminate birds, fish, and drinking water. Left in the medicine cabinet, they can be stolen by criminals or abused by children and teens. Maine has the oldest population in the country — a source of drugs — and a serious prescription drug problem, particularly in rural areas.
Takeback programs aim to provide a safe, secure and anonymous way for people to dispose of unused and unwanted drugs. Since 2010, the DEA has sponsored five national “takeback day” events and paid for disposal of the collected drugs. In Maine, drugs turned in to collection boxes at police stations have been handed over to DEA on takeback days for disposal.
DEA will sponsor another takeback day — possibly its last — on April 27.
NEW POLICIES ON DRUG DISPOSAL
DEA drug-disposal funding is widely expected to end later this year, shifting disposal costs back on local and state authorities. In expectation, Gov. Paul LePage last year created a prescription drug abuse task force whose duties include developing disposal solutions.
According to Greg Couture, assistant to the commissioner for public safety, the task force is entirely funded by a $60,000 grant from the Pharmaceutical Research and Manufacturers of America. PhRMA successfully opposed a 2010 bill that would have required its member drug companies to fund Maine’s drug takeback programs.
State Environmental Protection Commissioner Patricia Aho, who chairs the task force’s disposal subcommittee, has reinterpreted disposal rules to allow collected drugs to be treated as household waste rather than hazardous waste. The shift paves the way for the drugs to be burned at municipal waste incinerators in Portland, Auburn and Orrington, rather than being sent out of state for disposal in more permissive locales or by hazardous waste combustors.
In a January 2012 memo, Aho wrote that because the collected materials “would amount to less than 5 percent of a load” at the municipal waste plants, “we do not expect incineration of medications to have a measurable effect on emissions or ash characteristics” at the facilities. She also said the plants “achieve a 99.99 percent destruction efficiency of combustion by-products.”
This represents a shift from the Department of Environmental Protection’s previous interpretation of the rules, which was articulated in an August 2011 memo written by Maine Assistant Attorney General Nancy Macirowski. Medications, she noted, can contain hazardous substances and therefore are “deemed to be a hazardous waste.” Drugs disposed of by households are specifically exempted, but not when “collected in an ‘unusual quantity’ such as at a collection event.”
“As things now stand, there is not any solid waste disposal facility in Maine approved by the DEP to accept unsorted pharmaceutical waste,” Macirowski wrote.
Michael Wardrop, the head agent at the DEA’s Portland office, said the old interpretation “put the wall up” against in-state incineration of unsorted drugs.
The new interpretation holds that loads of several hundred pounds of drugs do not constitute an “unusual quantity” under the rules, on the grounds that they represent a tiny percentage of the municipal waste plant’s hourly burn load. As a result, they can be categorized as household waste.
EFFECTS ON AIR QUALITY DEBATED
A review of hundreds of pages of department files and interviews with a dozen sources involved in the issue suggested there is a difference in opinion between air quality experts (whose data supports the changes) and solid and hazardous waste specialists (who remain concerned about whether the substances will be fully destroyed).
Marc Cone, director of the DEP’s Bureau of Air Quality, notes that air emission tests for dioxin and other relevant substances recently conducted at the ecoMaine incinerator in Portland suggest that any drugs presently in the household waste stream are being cleanly burned. The department hasn’t been able to test the effect of several hundred pounds being burned but plans to do so with some of the drugs collected during the DEA’s April 27 takeback event.
“It’s very evident that the combustion that occurs in these units is very good,” Cone said. “I can’t imagine the tests in April will result in anything different.”
Solid waste experts at the DEP appear to have had reservations about the proposed shift, according to internal emails obtained through a public records request.
“My understanding is that the significant difference between hazardous waste incineration and solid waste incineration is not in the emissions control technology, but in the incineration technology, the control of the feed rate for different materials, and the burn temperature monitoring and control,” Carole Cifrino, manager of product management programs, wrote a colleague in the air bureau in November 2010. “If the pharmaceutical companies think that solid waste incineration is achieving the desired results, why aren’t they stepping up to do the testing and demonstrate it’s safe?”
Others expressed concern about the lack of data.
“Nobody seems to be able to cite any emission studies for pharmaceuticals (at municipal plants),” another DEP product stewardship expert, Ann Pistell, wrote colleagues in November 2011. “The science in which to base public policy seems alarmingly absent to me.”
In a written statement to the Press Herald, the U.S. Environmental Protection Agency said, “EPA is not aware of any available emissions data on the efficacy of burning pharmaceuticals in a municipal waste combustor” because “it is impractical and not cost effective for an incinerator to ever burn a load consisting only of waste pharmaceuticals.”
“The concern with pharmaceuticals is that even a small amount of some of the persistent agents don’t completely combust, they can leak out, and they have very small thresholds where they can have an effect,” said toxicologist Melinda Treadwell, provost of Keene State College in New Hampshire.
Because of the lack of data, the EPA recommends that takeback programs dispose of unwanted medications “in a permitted hazardous waste incinerator or cement kiln.” As a fall-back position, it recommends that they be burned in municipal incinerators, as this is safer and cleaner than other alternatives: having people throw them in landfills with their trash or flush them down their toilets.
Currently, collected drugs are being burned at a municipal waste plant in Haverhill, Mass., under an environmental waiver negotiated by the federal DEA, according to Wardrop, the head agent in Portland.
If federal funding for takebacks ends, that option would likely evaporate, he said, potentially leaving state and local law enforcement with disposal costs of up to $5 a pound at an out-of-state hazardous waste facility.
Burning drugs at municipal waste plants would likely be much cheaper, Wardrop said, about $80 a ton, or 4 cents a pound.
Stevan Gressitt, founding director of the University of New England Institute for Pharmaceutical Safety, who sits on the drug task force, says the cost of inaction is even greater.
“Addiction is causing overdoses and pharmacy holdups and drug-driving events,” he said. “I would propose you have far more dead people in the state of Maine as a direct result of the availability of these drugs than we would ever have from putting them in a incinerator.”
Staff Writer Colin Woodard can be contacted at 791-6317 or at:
cwoodard@pressherald.com
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.