BINGHAM – Getting to this small town along the Kennebec River can take some time. About 23 miles north of Skowhegan, it is a half-hour drive up U.S. Route 201, winding along the river on a road other drivers share with logging trucks.
The high school has 66 students, and there are just two restaurants.
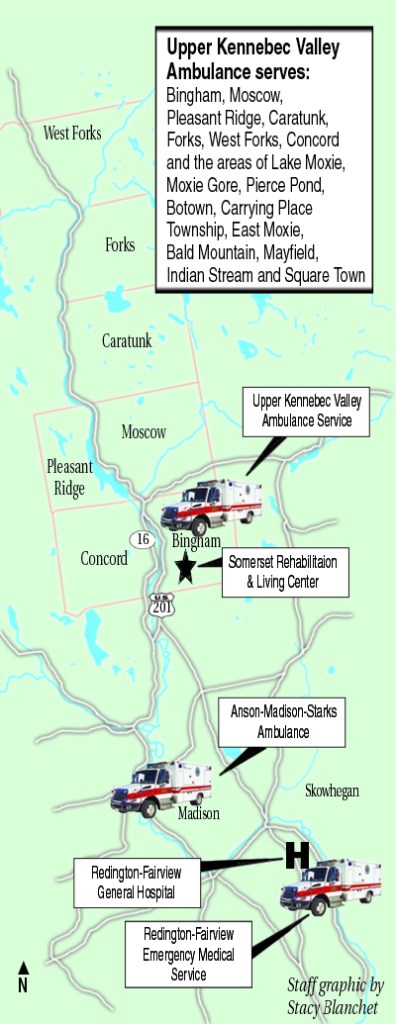
The town also is the base for the Upper Kennebec Valley Ambulance Service, which attends to people in six towns and 11 unorganized townships in northern Somerset County. As in many rural areas in Maine, services such as the ambulance are shared among communities.
Trying to figure out how to pay for shared services can be a challenge in rural communities.
While facing rising costs, the ambulance service here is considering changing the way it is paid in the communities it serves. Yet because the area’s population is so small and spread out, the cost of services is higher than in other local districts. In those areas, services can be shared at lower costs to taxpayers or provided by hospitals or private companies.
HIGH COST IN A RURAL AREA
Communities that use Upper Kennebec Valley Ambulance pay based on their population, with residents in Bingham paying about half the money collected. Some think the way costs are shared is unfair because Bingham has a nursing home, which accounts for many of the calls, and other areas with smaller populations rely on the ambulance service more heavily during tourist seasons.
In Bingham, residents recently voted down a request from the ambulance service for $69,990, about 40 percent of the service’s total budget, for 2013. Instead, local voters opted at the annual town meeting to give $35,000.
As a result, the service has only enough money to operate through June, said Marlene Merrill, president of Upper Kennebec Valley Ambulance’s board of directors.
Bingham First Selectman Steve Steward said: “They provide a good service, but I think many people feel the upper river towns are not contributing what they should be to the cost.”
In 2012, the service made 253 calls in Bingham, 97 of which came from Somerset Rehabilitation & Living Center, said Tim Pomelow, the service’s executive director.
“They incorporate that number into Bingham’s cost, but there are people from everywhere in that nursing home,” Steward said.
Other towns rely on the service more heavily during tourist seasons, he said.
“About 85 percent of properties upriver are camps. They aren’t included in the population, but they still use the service,” he said.
Steward said the area needs and wants to keep the service, but the cost is too high.
In 2012, Bingham contributed $88,544 to the service’s annual budget of $214,627, as well as an extra $12,000 to address a financial shortfall.
Steward said a special town meeting was held to approve giving the additional $12,000 to the service, which ran out of money at the end of 2011.
“They were on the verge of collapse, and we had to bail them out,” he said.
Merrill said operating costs have increased, primarily because of the prices of fuel, equipment and insurance.
The service added 24-hour paramedic coverage in August. Before that, Pomelow said, paramedics had been on duty about 80 percent of the time. The new staff includes one critical-care paramedic, the highest level of care available; three other paramedics, and three emergency medical technicians, he said.
“People don’t understand that it costs money to have these things. Last year there were some days when there were just no paramedics on duty. Now there is someone there every day,” Merrill said.
Steward said he likes the service’s quality, but the cost seems too high to some residents.
“At some point you have to say, how much is too much to pay?” Steward said.
SHARED SERVICES COMMON
Shared services such as fire and ambulance are common statewide, especially in smaller towns and more rural areas, said Maine Municipal Association spokesman Eric Conrad.
“Municipal collaboration has been going on for many decades, but there is no law or local ordinance about how to pay for shared services,” he said.
Merrill said the service is considering three new formulas for municipal payments to complement the revenue they collect from insurance.
• Charging a rate based on a community’s population plus a percentage of the per-capita cost for each seasonal unit.
• A variation of that formula calls for a higher base rate.
• Charging communities based on their usage of the ambulance over the previous five years.
The service has based its formulas on research into what other Maine towns do, she said, although the upper Kennebec Valley area is a little different because of its small population.
DELTA AMBULANCE: A NONPROFIT
Delta Ambulance, with offices in Waterville and Augusta, serves 17 communities, from Whitefield in the south to Rome in the north. Delta, a nonprofit, responds to about 17,000 calls per year, said Bill McKenna, director of community relations.
The service is paid for based on the work provided, he said.
“We do a call, treat and transport a patient, and the call is paid for by the patient’s insurance,” said McKenna.
It takes about 2,000 calls to generate enough insurance revenue to support an around-the-clock ambulance staff for a single truck, he said.
Last year, Upper Kennebec Valley Ambulance responded to 471 calls, a record year, according to Pomelow.
“To staff an ambulance, you have to pay for the truck, gear and people. In a small-volume service, that money has to come from somewhere,” McKenna said.
Delta does not charge anything to the municipalities it serves, but McKenna said that in smaller coverage areas there may be no other option. Money can be saved by using volunteers, but even then, the cost of the truck, insurance, diesel fuel and other expenses adds up, he said.
“It’s a terribly expensive business,” McKenna said.
REDINGTON-FAIRVIEW EMS: HOSPITAL-OWNED
Redington-Fairview EMS operates out of Redington-Fariview General Hospital in Skowhegan and is owned by the hospital, so the communities it serves do not have to pay subsidies, director Barbara Demchak said.
The service, though, still collects insurance revenue for each call, she said.
It responded to 4,526 calls in 2012 and provides mutual aid to the upper Kennebec Valley.
“If dispatched, we will respond if crews are available. But it is a significant distance to Bingham, and folks beyond are an even greater run,” she said.
The ambulance can charge a per-mile cost beyond the base rate, but only after it has the patient in the vehicle, she said.
The cost to the patient would not differ too much because he or she still would still be going to the hospital in Skowhegan, but the extra time to send an ambulance from Skowhegan could make a difference in the care they receive.
“A majority of calls are not life-or-death, but there are some that force you to ask, what is the cost to the patient’s condition if there is no ambulance close by?” Demchak said.
It’s a good idea for rural communities to have a contingency plan if they don’t have 24-hour emergency care available, she said. For example, the local Fire Department could keep an automatic defibrillator to help someone having a cardiac arrest.
“The ability to provide electric shock can save someone’s life, and you don’t need a paramedic to administer it,” she said.
ANSON-MADISON-STARKS AMBULANCE: SHARED SERVICES
The Anson-Madison-Starks Ambulance is an example of a shared service that is supported by town subsidies and insurance revenue. Each town pays $15 per capita based on the last census, said director George Demchak, brother of the Redington-Fairview EMS director.
In 2012, the ambulance service responded to 1,633 calls, he said. Madison paid $72,825, about 41 percent of the subsidies collected; and the service responded to 668 calls there, he said.
“Upper Kennebec Valley is in a different situation, because they don’t get that many calls. They don’t get that much income from insurance revenues,” he said. “It’s a tough situation because you want what’s best for people, but somebody has to pay for it.”
FINDING THE BEST OPTION
If the Bingham-based ambulance service closes, residents would have to rely on Anson-Madison-Starks or Redington-Fairview EMS.
The area is home to many elderly people, including those at the nursing home in Bingham, who rely more heavily on emergency care, Merrill said.
“It would be a hardship for these towns not to have an ambulance,” Merrill said. “Hopefully, we can figure out a situation that is agreeable to everyone.”
Steward said he doesn’t foresee the service going away, but there needs to be a solution to how it is financed.
“It really is quality care and something that we need,” he said.
Rachel Ohm can be contacted at 612-2368 or at:
rohm@mainetoday.com
Copy the Story Link
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.