Daniel Vassie Jr.’s road to addiction began like so many others: A doctor prescribed him painkillers to treat a bad back. Before long, his body craved more than his doctor would provide.
“I sought it out myself on the street,” he said. “I couldn’t go without.”
Vassie stayed with pills for a while before graduating to heroin for two reasons: It was cheaper and easier to get.
“I said I’d never touch it,” he said. Yet there he was shooting up. Selling to others just to support his habit. Spiraling downward.
Vassie, 36, of New Gloucester, knows he’s lucky. He could easily have been one of the growing number of heroin overdose deaths hitting Maine over the last few years – 28 in 2012, up from seven deaths the year before. He also attempted suicide more than once before steering toward recovery.
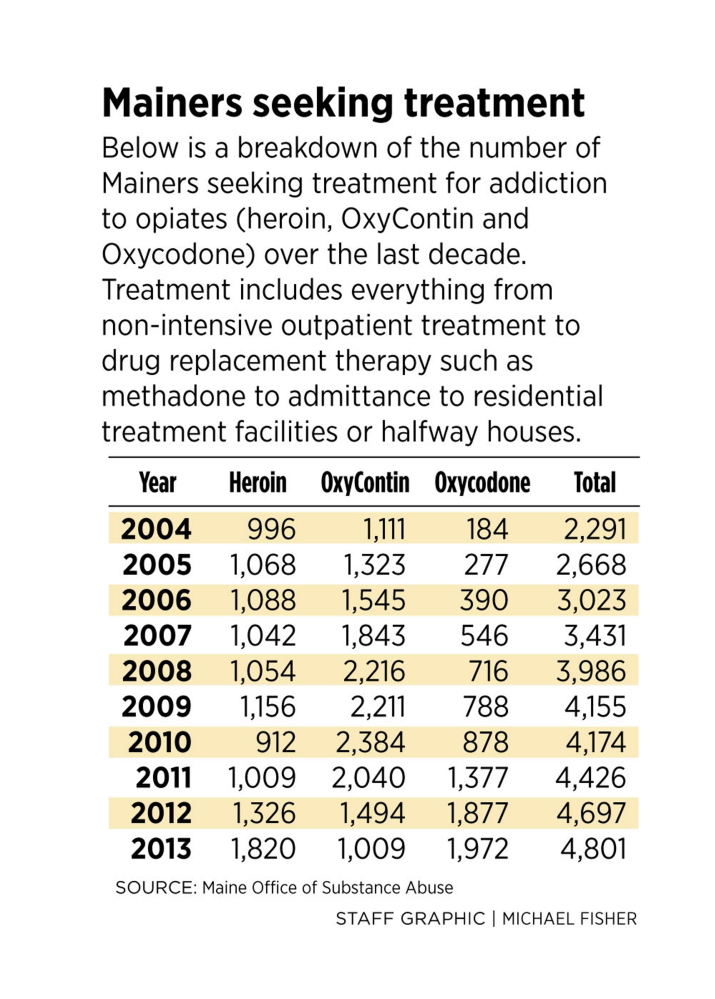
The number of people in Maine like Vassie seeking treatment for opiate abuse has more than doubled in the last decade, to about 4,800 in 2013. In the last three years alone, demand has increased 15 percent. The number seeking treatment for heroin abuse has doubled since 2010, to 1,820.
Yet even as demand for treatment surges, funding has not kept pace. The number of beds available for inpatient drug treatment, already low to begin with, hasn’t changed in years.
In 2010, Maine spent a total of $47 million on substance abuse treatment ranging from sober-living situations such as halfway houses, to outpatient counseling, to hospitals or short-term stays in rehabilitation clinics. Last year the amount dropped by 7 percent, to $43.7 million. The state’s share of a federal block grant for treatment and prevention also decreased from $6.7 million to $6.3 million in that period.
That $47 million still represented only 3.4 percent of the $1.4 billion total estimated cost of drug and alcohol abuse in Maine, including medical, criminal and incarceration costs.
Those who have been able to get into treatment often trade heroin for methadone or suboxone, synthetic versions of opiates that do not provide a high but allow addicts to avoid sickness from withdrawal. While they are not considered treatment on their own, methadone and suboxone are supplemented with counseling to address the addiction itself.
Vassie is in counseling and has used suboxone since 2009, but he doesn’t know how much longer he can stay on it.
As of Jan. 1, Vassie was booted off MaineCare, the state’s equivalent of Medicaid, because he is a “noncategorical,” meaning he has no children and no illness debilitating enough to warrant taxpayer-funded health insurance.
Maine decided to stop covering some childless adults to help curb the costs of MaineCare, removing 19,000 people from the program. In 2012, the most recent year for which data were available, 869 of those people were using MaineCare to pay for methadone treatment for heroin addiction. Many more likely were receiving suboxone, although the state does not keep those numbers.
Substance abuse professionals largely agree that inpatient residential care works best for opiate addicts. But the number of beds available for substance abuse rehab in Maine is slightly less than 200, enough for fewer than one-half of 1 percent of the 4,800 people seeking treatment for opiates last year. The number of beds has not changed over the years, even as the need has risen.
Those who work in substance abuse treatment say decreasing funding is the wrong approach, and paying for more treatment is cheaper in the long run.
“There is no question there is a return on investment,” said Guy Cousins, director of Maine’s Office of Substance Abuse, which estimates that every dollar spent on treatment saves as much as $5 in health care costs.
But it is difficult to persuade states to spend more.
Sue Foster, director of policy research and analysis for the National Center on Addiction and Substance Abuse at Columbia University, said it’s hard for people to see the value in supporting others’ poor choices.
“So we keep chasing the drug of the day. Right now, it’s heroin,” she said. “We’re focusing on the drug but not the addiction.”
Vassie understands taxpayers might balk at paying to help addicts recover. He also knows that without treatment, he could end up using heroin again.
His family is helping pay for his suboxone since he lost MaineCare coverage, and his counselor has been meeting with him for free.
“But I don’t want people out there thinking we’re not people,” Vassie said. “I’m a person. I have a name.”
ENFORCEMENT VERSUS TREATMENT
Gov. Paul LePage, in his State of the State address this month, addressed Maine’s drug problem and offered his solution for how to combat it.
“While some are spending all their time trying to expand welfare, we are losing the war on drugs,” he said.
LePage’s response was to beef up enforcement, proposing four new drug prosecutors; four new judges for drug courts in Portland, Lewiston, Bangor and Presque Isle; and 13 additional positions in the Maine Drug Enforcement Agency.
There is an argument to be made for more positions: In 2013, the MDEA investigated 223 heroin cases, more than triple the number in 2011. By contrast, the number of investigations involving synthetic drugs decreased from 386 to 294 in that time.
In fact, one of the reasons heroin has seen a resurgence is because police have begun to crack down harder on abuse of synthetic opiates such as OxyContin and oxycodone.
The growing number of people using heroin in Maine mirrors a national trend. A recent Substance Abuse and Mental Health Services Administration survey found that between 2007 and 2012, the number of heroin users nationwide increased from 373,000 to 669,000. The recent death of actor Philip Seymour Hoffman from a heroin overdose has also put an additional spotlight on the drug’s resurgence.
LePage’s focus contrasts sharply with that of Vermont Gov. Peter Shumlin, a Democrat, who devoted his entire State of the State address to his state’s growing drug problem, and calling for more treatment funding.
Some would like to see LePage take a similar approach.
Rep. Ann Dorney, D-Norridgewock, has been a physician for 31 years and has spent most of the last decade dealing with substance abuse.
“I can see why people want to save money,” she said, about eliminating MaineCare coverage for childless adults. “People are convinced that you just get sober and you’re better. Opiates are not like that. Five percent of people can just stop cold turkey. Most can’t.”
Mainstream trends in public policy have begun to tilt toward addiction intervention and treatment as a more effective response; LePage’s record – and that of the Legislature – has been mixed on the issue.
In early 2011, LePage proposed $4.4 million in cuts to substance abuse treatment funding, a nearly 10 percent decrease. He later reduced that by half, but lawmakers instead restored all of the funding.
In July the same year, LePage visited Serenity House, a halfway house in Portland for men receiving addiction treatment, calling its program a model. Serenity House, however, was one of 10 facilities that would have likely closed had his cuts taken effect.
Last July, LePage directed $50,000 from his emergency contingency fund to a drug treatment center in Ellsworth that works with the local drug court program. Drug courts allow participants facing criminal charges to avoid jail time if they enter treatment and submit to testing, an approach that advocates say is better for addicts because they would likely not receive treatment in prison.
Drug courts have been effective in Maine: In 2010, 62 people graduated for a rate of 61 percent – higher than the national average of 48 percent. The re-arrest rate for all participants was 16.5 percent, compared to a rate of 33 percent for all criminal offenders.
But the drug courts cost money, too. They are funded through the Fund for a Healthy Maine, the state’s share of tobacco settlement money, but there have been attempts in recent years to divert those funds elsewhere.
“I think the Legislature and our state needs to be comfortable that there is a cost associated with prevention services, just as there is a cost associated with abuse,” said Peter McCorison, vice president of the board of the Maine Association of Substance Abuse Services and chairman of the governor’s Substance Abuse Services Commission.
Maine lawmakers also recently imposed a two-year cap for methadone and suboxone treatment. Dorney, however, said that someone trying to wean himself off methadone or suboxone in a short period of time is almost certain to relapse.
“Yes, it is just substituting one narcotic for another, but if you’re an addict, you have permanently changed the makeup of your brain,” she said. “It’s like emphysema. If your lungs are damaged, you’re not going to reverse that even if you stop smoking.”
Cousins, LePage’s top substance abuse counselor, said drug-based therapy has been proven to work better than abstinence, but it needs to be coupled with behavioral therapy.
“Providers are seeing considerable wait lists,” Cousins said. “The need is greater than the resources we have.”
The worst possible scenario is an addict reaching the point where he is ready for treatment and being told he has no place to go, Cousins said.
WHERE THE FUNDING GOES
The quickest and cheapest form of substance abuse treatment is detox, in which someone is admitted for a short period of time to a facility to rid the body of an addictive substance. Detox has proved to be an ineffective treatment for opiate addiction. Instead, most opiate addicts are offered drug replacement treatment with methadone or suboxone, which block the neuroreceptors in the brain in the same way heroin does.
In 2013, 1,820 Mainers sought treatment for heroin addiction. Of that total, 40 percent received methadone while half received some form of outpatient therapy.
Only 144 were admitted to hospitals as inpatients, while the rest went to rehab facilities, halfway houses or found other forms of treatment.
The best option, professionals say, is long-term treatment with drug replacement therapy. Dorney said 30 days of inpatient therapy, followed by at least six months in a sober-living environment, is ideal.
But MaineCare and many private insurance plans often do not cover inpatient treatment.
Patients who do get into residential treatment centers are lucky, given the small number of beds and the long waiting lists.
According to the Office of Substance Abuse, the state has 194 substance abuse beds – only 21 of them designated for women – and that number has not risen in several years, Cousins said. Sixty-seven agencies provide outpatient services ranging from methadone clinics to counseling practices, with only 16 of them also providing intensive outpatient care.
Services are available to those who can pay for it on their own: Earlier this year, Crossroads Back Cove in Portland, one of the few halfway houses for women in Maine, closed after losing $330,450 in funding from the state Department of Health and Human Services. A self-pay, 30-day residential rehabilitation center for women with private insurance or who can pay out of pocket opened in its place.
Phil del Vecchio, a licensed drug and alcohol counselor at SMART Child & Family Services in Windham, which offers substance abuse counseling, said the biggest problem in Maine is the lack of inpatient treatment.
Steve Danzig, a licensed drug and alcohol counselor in Windham, refers his clients out of state for inpatient treatment because there are far fewer options in Maine.
Danzig knows plenty about addiction. He’s been a counselor now for more than decade and has been in recovery himself for 16 years. Danzig progressed through many different drugs before finding heroin. His rock bottom came when he was living at a train station in New Jersey.
“There was a moment where I was standing near the train platform and I was ready to step in front of that train,” he said.
Instead, Danzig called for help. He made his way to Maine and got clean at Serenity House. Then he went back to school to help others. When he meets with clients and sees their desperation and hopelessness, he remembers his own experience.
He has a wife and three kids and a stable life but said he has to work at it every day.
“My drug addiction seems like a lifetime ago but it’s also fresh. The disease is still there,” he said. “It doesn’t take time off.”
Danzig said he joined a state task force a few years ago that was convened after Maine policymakers decided to aggressively address the state’s prescription drug problem, but stopped participating when he saw the direction it was headed. A 2012 report by the task force identified four core initiatives: drug collection and disposal; diversion alerts; education; and prescription monitoring. The focus was almost entirely on attacking the supply of drugs.
That approach has worked to an extent. The number of narcotic prescriptions filled in Maine decreased from 1.39 million in 2010 to 1.08 million in 2012, the last year for which figures are available.
But it does not address demand.
Opiates change your brain, Danzig said. Sometimes irreversibly. That is the reason substance abuse professionals use methadone and suboxone to maintain someone’s brain function during treatment for addiction. Sometimes, a patient has the dose tapered gradually until it’s no longer needed, but that timeline varies depending on the severity of addiction.
One area where the increase in heroin use has been seen most is enrollment in the state’s needle exchange program. Needle exchanges allow drug users who inject to drop off dirty needles at one of five approved locations in exchange for new, clean needles. The programs operate without state or federal funding.
In 2010, 1,548 people were enrolled in the program. That number jumped to 4,333 in 2013, and the number of needles exchanged increased from about 160,000 in 2010 to more than 500,000 in 2013.
Needle exchange programs have been controversial for years but advocates say they are a proven way to help combat infectious diseases such as HIV/AIDS and hepatitis and they get dirty needles off the streets.
And, needle exchange can lead to treatment. In 2013, Maine’s needle exchange providers referred 372 clients for treatment.
ADDRESSING THE STIGMA
Sayra Small of Durham wants to see better access to drug treatment because it saved her life.
She will be three years sober in March, but it took her more than a decade to get there.
She started when she was 19, discovering OxyContin and oxycodone while working at a restaurant in Bar Harbor.
Small used both off and on for years. But once those got too expensive, she switched to heroin. The needle didn’t scare her.
“If I was going to be bad, I was going to be the worst,” Small said.
She saw friends die from overdoses and others contract diseases from dirty needles. Even that didn’t stop her.
“What people don’t understand is: Drugs were not my problem,” Small said. “Life was my problem. Drugs were my solution.”
Her initial attempts at treatment failed. She didn’t have insurance, didn’t qualify for MaineCare and couldn’t afford more than suboxone treatment, which didn’t address the root cause of her addiction. Small said she never was good at facing the problems in her life and drugs made them go away.
When she enrolled in an intensive outpatient treatment program in 2010, the bills piled up, unpaid.
Then, in January 2011, she found out she was pregnant.
“I just decided that even if I never got the chance to raise that child, I was going to make sure it was healthy,” she said. “I was going to give it a chance.”
Her pregnancy made her eligible for MaineCare, and she signed up for WIC, food stamps and counseling. She was prescribed subutex, a form of suboxone that is safer for pregnant women.
Small said when she was admitted to the hospital to deliver her baby, she was treated like a junkie, not like someone who was trying to get clean. She said hospital workers didn’t understand that she was in treatment, that she was trying to get better for the baby.
“That’s one of the reasons I feel as strongly as I do about speaking out,” she said. “Like people don’t feel guilty enough without that stigma.”
Small, now 34, stayed clean and kept her child, now a healthy 2-year-old. She works at Opportunity Alliance in Portland, which coordinates nearly all of the region’s social service needs, and sees people every day who are where she used to be.
She also no longer receives public assistance. She still takes suboxone but pays for that herself because, as she says, “Why mess with it?”
“I’m killing it right now,” she said. “My life is great, I have a great job, I have a husband and son. Why would I chance relapsing if this helps me?”
Send questions/comments to the editors.







Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.