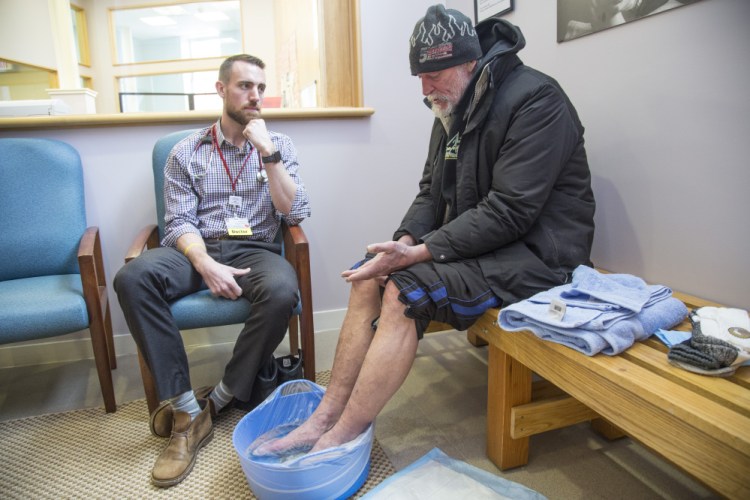
Brian French lumbered into the health clinic at 20 Portland St. on a frigid winter afternoon. Within minutes, the 56-year-old took off his shoes and socks and began soaking his frostbitten feet in warm water and Epsom salt.
Seated next to him was Dr. Adam Normandin, a family and internal medicine resident from Maine Medical Center who helps staff at the Portland clinic. The doctor simply listened to the man’s story, which at times was rambling and disjointed. Soon, Bill Burns of the Preble Street social services agency emerged with new socks and towels for the patient.
“Bill, I appreciate all the years you’ve been chasing me around,” French said. “You’re a beautiful man.”
French is one of the 75 clients of the homeless health clinic that opened Jan. 17 across from the Preble Street center. The clinic, once run by the city, had been closed since 2014 after the city lost its federal grant funding to Greater Portland Health, which at the time was called Portland Community Health Center.
But rather than using Greater Portland Health during the past two years, many of the chronically homeless have been going without medical care or visiting a hospital emergency department for treatment, homeless advocates say.
In announcing the reopening of the facility last month, officials said the Maine Med-Preble Street Learning Collaborative was seeking “to help fill the void left by the closing of the city of Portland Health Care for the Homeless Clinic in 2014, provide no-barrier access to health services, care-coordination and education, and create a new point of entry to the health system.”

Dr. Adam Normandin and nurse practitioner Samantha Doe discuss the case of a homeless man who recently came to the clinic with a life-threatening condition. Normandin and Doe say the clinic’s open and quiet atmosphere helps patients feel comfortable and welcome.
Preble Street Executive Director Mark Swann said Greater Portland Health has a talented clinical staff and high-quality health services, but it simply doesn’t offer the same amount of clinical hours, mental health or dental services that the city clinic once did.
If there wasn’t a gap in services, Preble Street and Maine Med would not have spent the past two years setting up this new program, Swann said.
“This is driven by what our clients tell us and what our social workers experience every single day,” he said. “There’s no question there’s much less available in terms of walk-in hours. And there’s no question there’s a much less robust mental health aspect to the care.”
Dr. Renee Fay-LeBlanc, chief medical officer at Greater Portland Health, said she’s not aware of any gaps in service. She notes that Greater Portland Health is now serving more homeless individuals than the city clinic did. She said her staff is working closely with the new collaborative, but she’s concerned about unintended consequences from having two organizations doing the same kind of work.
“We’re always going to welcome services for people who are vulnerable, but there is the potential of bad outcomes if there is a duplication of services or fragmentation of care,” Fay-LeBlanc said.
Until 2014, the city of Portland had operated Health Care for the Homeless at 20 Portland St. for 20 years. Preble Street owns the building and had invested $1 million in renovating the space for the clinic, which employed 36 people.
But the clinic closed after the city lost $680,000 in federal grant funding. The city had received the grant without competition since 2009, but in 2014 it made a clerical error in its application, prompting Greater Portland Health to apply in the second round. Greater Portland Health beat out the city, forcing the clinic to close.
Greater Portland Health opened a new clinic at 63 Preble St., right across from the Preble Street day shelter and soup kitchen.

Brian French thanks Bill Burns of the Preble Street center for bringing him new socks.
A MODEL FOR LEARNERS
The MMC-Preble Street Learning Collaborative offers no-barrier medical, counseling and case management services to high-risk people experiencing homelessness, while giving medical residents a unique opportunity to gain experience working with an underserved population.
One of the goals is to establish relationships with a hard-to-reach population and get them into a primary care facility, such as Greater Portland Health.
“This partnership aligns with MMC’s commitment to delivering innovative population health and affordable care services, as well as our three-part mission of caring for our community, educating tomorrow’s caregivers and researching new ways to provide care,” Maine Med’s chief academic officer, Dr. Peter Bates, said in a written statement.
Interest in participating in the collaborative is strong among medical residents, according to Maine Med.
“It’s the right thing to do – to care for the most vulnerable people in the community,” Dr. Normandin said, explaining his decision to serve his residency at the collaborative.
According to Maine Med, most of Portland’s homeless population lacks insurance and there is little access to emergency care, other than emergency departments. The hospital conservatively estimates that led to 1,481 avoidable hospital days in 2015.
The 8,400-square-foot facility at 20 Portland St. has three exam rooms, a reception area, consultation room, two showers, and office, conference and educational rooms. Clinical staff seeks to provide free walk-in care, mental health services, triage, urgent and follow-up care, wound care and substance abuse treatment, among other services.
The combination of medical residents operating in a quiet and supportive environment is more welcoming to people struggling not only with health issues and homelessness, but also substance abuse and mental illness, said Malia Haddock, program manager for Maine Med’s Homeless Health Partners, which provides case management services.
“We’re trying to slow things down – we call it slow medicine,” Haddock said. “It’s really focused on building a relationship with the patient from the start.”
Burns, of Preble Street, said that approach has already saved at least one life, when a veteran came to the collaborative after he was unable to see his primary care doctor. He visited an emergency department, but was discharged. Because he was still not feeling well, he went to 20 Portland St. After spending time with the man, nurse practitioner Samantha Doe realized he had a life-threatening condition and had him admitted at the emergency department.
“Having those quiet spaces, patients open up more and give you more symptoms,” Doe said. “Some patients at the ED are totally out of their element and they just want to get out of there.”
Were it not for the reopened clinic on Portland Street, French said he would not have sought care for his frostbitten feet.
“I would have just walked this off until I fell down,” he said.
But since he already had a relationship with Burns, he was comfortable getting help there.
“It was the kindness of a person,” French said, explaining his reason for going to the clinic. “You see a friend who doesn’t have to ask you nothing because he already knows what you need.”
Randy Billings can be contacted at 791-6346 or at:
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.