With one Mainer a day dying from a drug overdose, an antidote that could help friends and family save a loved one’s life sits out of reach on pharmacy shelves, stuck in a bureaucratic limbo created by Gov. Paul LePage and Maine’s pharmacy regulators.
The president of the Maine Board of Pharmacy says LePage must sign off on rules that would allow pharmacies to sell naloxone, a life-saving anti-overdose drug, to families or friends of opioid addicts without a prescription.
But Maine Attorney General Janet Mills says LePage has no legal role to play in the matter, and she urged the board to publish the rules with or without the approval of the governor, long an opponent of widespread distribution of naloxone.
The board unanimously approved the rules and sent them to LePage in August 2017. Five months later, there has been no action.
The governor’s press secretary, Julie Rabinowitz, said Thursday the rules were still “pending.” Two days earlier, LePage told a Sunday Telegram reporter who asked about the matter, “I don’t know a thing about it.”
Rabinowitz declined to provide further details about why the rules were being held up, and the pharmacy board president, Joseph Bruno, refused to comment.
A new law allows pharmacists to sell the life-saving anti-overdose drug to families or friends of opioid addicts without a prescription. A dose of the drug goes for between $50 and $75.
Under the law, the pharmacy board was directed to develop rules to guide pharmacists in responding to requests for naloxone, often sold under the trade name Narcan. The rules haven’t been promulgated, or published yet, so pharmacies have no guidelines for selling the antidote in a way that complies with the law.
“There is no legal reason why the pharmacy board can’t promulgate the rules,” Mills said Thursday. “There is nothing in the statute that requires the governor to sign off on the rules.”
Mills said it wouldn’t be fair to suggest the delay was leading to people “dying in the streets” but there was no reason to delay access to naloxone, which was twice approved by the Legislature. Lawmakers passed one naloxone bill over LePage’s veto, and a second bill became law without his signature.
“This is an expression of a clear public policy and it’s a shame it is being delayed,” Mills said.
It’s not known how many lives might have been saved if naloxone was widely available, but Maine emergency workers used it to revive patients 2,380 times in 2016 and 1,585 times in 2015, according to state figures. Data for naloxone use in 2017 have not been released yet.
Mills has used legal settlement funds to purchase naloxone for about 70 police departments around the state. Brian MacMaster, a chief investigator in Mills’ office, said the departments have used naloxone 350 times to save the lives of overdose victims.
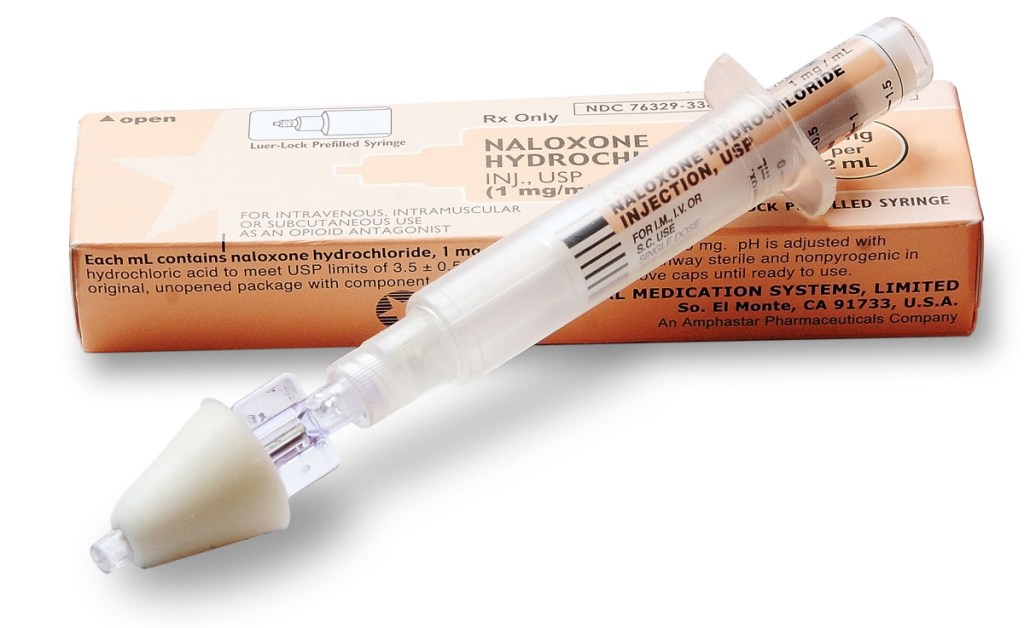
Naloxone can quickly reverse the effects of an overdose – such as arrested breathing – by attaching to the opioid receptors in the brain. It is typically given in a nasal spray or auto-injector pen.
MAKEUP OF PHARMACY BOARD
Maine reported 376 drug overdose deaths in 2016, more than double the number just three years earlier. The Attorney General’s Office has not finalized the numbers for 2017 yet, but Maine was still averaging more than one overdose death a day for the first six months of 2017.
At that rate, as many as 150 Mainers may have died of overdoses in the five months that LePage and the pharmacy board have been sitting on the naloxone rules.
Bruno, the pharmacy board president, owns the Maine-based Community Pharmacy chain and is a former Republican lawmaker who donated $4,750 to LePage’s campaigns for governor in 2010 and 2014. Other members of the pharmacy board declined to comment and referred questions to Bruno or the board’s administrator, Geraldine Betts, on Friday.
One member said he had been instructed not to talk to the press in case something got “misconstrued or I said something incorrect,” and another said the delay in the naloxone rule-making presented an “interesting dilemma.”
The board includes two public representatives and four pharmacists who represent both large chain pharmacies and smaller community pharmacies. Members serve three-year terms and all the current members are LePage appointees.
Betts, the board administrator, did not respond to a request for comment Friday on why the board sent the rules to LePage for approval.
Pharmacies make their own decisions
With no guidance on how to carry out the naloxone law, pharmacies are left to make their own decisions.
Hannaford, which operates 52 pharmacies at its grocery stores in Maine, said its pharmacists would not dispense Narcan without a prescription until the rules are finalized by the state.
“We are providing that medication by prescription in our stores until the rule-making process for over-the-counter sales is complete,” Eric Blom, a Hannaford spokesman, wrote to the Sunday Telegram via email Friday. “While that process continues, we would not have additional comments around this.”
CVS said last week that it, too, will not provide naloxone without a prescription until the state’s rules are published. Walgreens, another chain pharmacy in Maine, has said it will provide the medication without prescription, under a standing order it has from a physician to do so, as it does in 45 other states where it operates.
Maine’s decision to allow the antidote to be dispensed without a prescription mirrors that of states around the U.S. that have adopted similar policies. In all, 48 states allow the medication to be dispensed without a prescription, some under laws like Maine’s and some under a statewide standing order of a state medical director.
According to a report published in Kaiser Health News, some are questioning whether there is even demand for the antidote in the marketplace while others say the public has not been made fully aware that it can get naloxone without a prescription. In the report, other pharmacists said they were reluctant to take on a new responsibility and voiced concerns over new expenses.
But advocates for the policy, including Talia Puzantian, a pharmacist and associate professor of clinical sciences at Keck Graduate Institute School of Pharmacy in Claremont, California, said the wide distribution of pharmacies in the U.S. made them the ideal place to help educate the public on overdose prevention and treatments.
Puzantian said in a Telegram interview that it’s likely true there is not a lot of demand for naloxone from friends and family of those at risk of overdosing.
“But that’s because people don’t know about it,” she said, adding that just as pharmacies have a role to play in the distribution of prescribed opioid medicines, they should also play a role the distribution of the antidote, in case it is needed.
LEPAGE’S LONG-STANDING OPPOSITION
Maine’s opioid crisis was the focus of a 10-day Portland Press Herald/Maine Sunday Telegram series that examined the soaring death rates, the lack of treatment options, and the toll taken on families and communities.
LePage has been a staunch critic of the regular or repeated use of naloxone, saying it creates a false sense of security and encourages addiction, angering some in the drug treatment community with what many consider to be inaccurate statements about the use and need for the antidote.
“Naloxone does not truly save lives; it merely extends them until the next overdose,” LePage wrote in the 2016 letter in which he vetoed a naloxone bill. “Creating a situation where an addict has a heroin needle in one hand and a shot of naloxone in the other produces a sense of normalcy and security around heroin use that serves only to perpetuate the cycle of addiction.”
In May 2016, LePage told a Lewiston town hall audience that a student in Portland’s Deering High School had been treated with naloxone three times in one week and on the third time came to and went back to class. The story was rebutted by then-acting superintendent of schools Jeanne Crocker, who said it never happened.
In 2017, LePage also unsuccessfully proposed legislation that would have required those who receive repeated doses of naloxone to pay for it. The governor has also told town hall audiences that Maine’s overdose crisis would finally end once the current generation of addicts are all dead.
The Legislature originally approved making naloxone available over the counter in April 2016 and easily overrode a LePage veto. But the Board of Pharmacy sent the issue back to the Legislature because members said some aspects of the language crafted by lawmakers were unclear.
An amended bill passed both the House and Senate with overwhelming support – unanimously in the Senate and on a 126-20 vote in the House – last June and became law without the governor’s signature.
NALOXONE OFFERS A CHANCE AT RECOVERY
Maine’s law was intended to allow a friend, family member or somebody who lives with a person suffering from an opioid substance use disorder to obtain the overdose kit, which usually consists of two doses of naloxone that can be administered by a nasal mist, to have on hand in the event of an overdose.
Like laws in other states, Maine’s law would require pharmacists to participate in an approved two-hour training course in order to be able to dispense the medication, according to the draft rules.
Democrats as well as Republicans hoping to replace LePage in 2018 have said they support the policy of allowing the friends and family members of a potential overdose victim to have access to naloxone without a prescription and have urged the governor to either explain the delay or move the rules forward.
Puzantian, the California pharmacy professor, said she has heard others make the same argument as LePage, that naloxone availability will somehow enable – if not promote – more drug use.
“There is a large portion of the public that feels by giving them the naloxone they are going to go out there and sort of Russian-roulette and use more than they would and just overdose and then just give themselves the reversal, but that’s not how it works,” she said. “You don’t give yourself the reversal, someone has to be there to give it to you.”
She sees each overdose as “an opportunity to intervene and provide treatment,” noting that if people die from an overdose there’s no opportunity for them to ever make it to recovery.
Puzantian also pointed to clear evidence, especially in New England states like Massachusetts and Rhode Island that have moved toward broader access to naloxone, that emergency room visits for opioid overdoses are decreasing.
“It’s hard to imagine the arguments people have (against this policy),” Puzantian said. “If it were their family member, … it doesn’t make sense to me.”
Scott Thistle can be contacted at 713-6720 or at:
sthistle@pressherald.com
Twitter: thisdog
Send questions/comments to the editors.




Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.