MBANDAKA, Congo — Irene Mboyo Mola spent 11 days caring for her husband as he died of Ebola in a hospital where she said nurses were too scared to get close. She helped him to the bathroom, picked up his feverish body when he lost his balance, and reinserted an IV that fell out of his bleeding arm.
“He told me all he could see was death,” said Mola, a 30-year-old mother of six, as she sat slumped on the floor in her small hut.
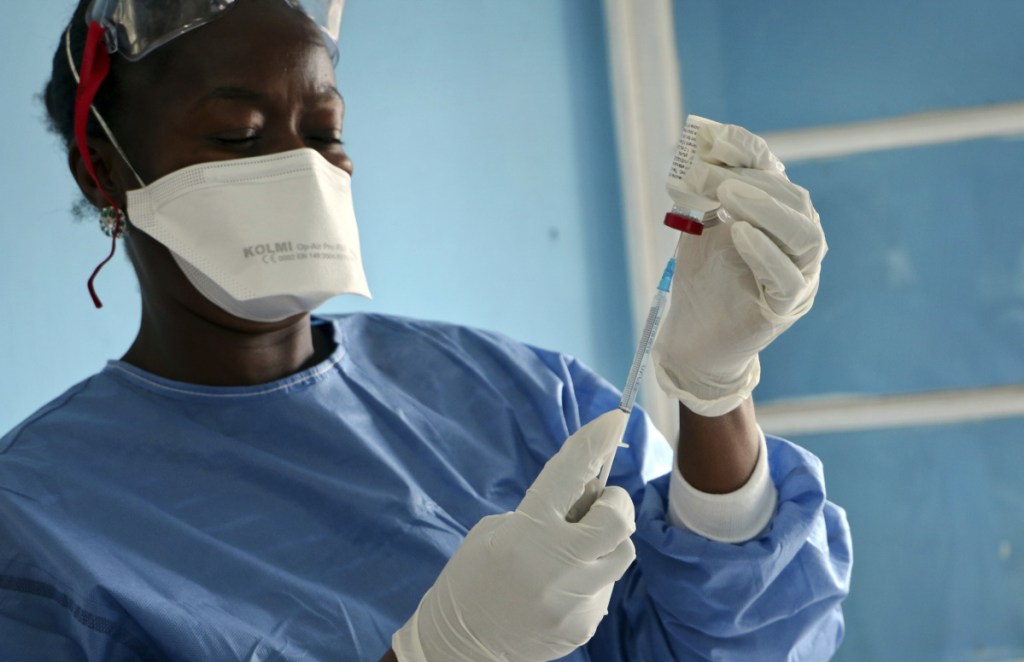
That close contact put Mola at high risk of getting a disease that has no cure and kills about half of those infected. But now, as Congo battles the most serious Ebola outbreak since the devastating 2014 epidemic in West Africa, health workers have something new to offer: a vaccine.
With thousands of doses dispatched to front-line health workers, the world is watching to see if a promising but still experimental vaccine might help stop this terrifying disease faster than traditional measures doctors have tried since Ebola was identified 40 years ago.
Even if the vaccine helps, there are serious hurdles. The shots must be transported deep into forests with few paved roads without it spoiling in the heat. Health workers have to identify and track down anyone who’s had contact with a sick person. Hardest of all, they must persuade a scared and wary population that shots pushed by foreigners could save their lives.
“Communities themselves must be at the center of the response if the activities are going to be effective,” said Jonathan Polonsky of the World Health Organization, a surveillance coordinator in Mbandaka, a city of more than 1 million in northwestern Congo.
Mola’s six children have all been vaccinated. But she refused, telling government social workers and WHO workers that she didn’t believe her husband died from Ebola. She said the hospital never showed her records confirming he’d tested positive for the virus.
FEAR AND OPPORTUNITY
There’s no guarantee the long-sought vaccine will help stop the outbreak. But Congo’s health ministry and the WHO rushed in 7,500 doses, created by the Public Health Agency of Canada and owned by Merck.
It was deemed the best option because the vaccine was found highly promising in testing a few years ago, when the epidemic in West Africa, which killed more than 11,000 people between 2014 and 2016, was starting to wane.
The plan: What’s called “ring vaccination,” to find and vaccinate everyone who’s had direct contact with a sick person – the first “ring” – and then contacts of those people, too, to break the chain of infection.
SPEED IS OF THE ESSENCE
Success with the vaccination strategy hinges on the speed at which health workers can identify people at risk. “If you detect cases late, you’re missing the opportunity to protect people,” said Dr. Iza Ciglenecki, who is working on the vaccination campaign with Doctors Without Borders.
Congo’s current outbreak has killed 14 people so far, according to the country’s Ministry of Health. There have been 38 confirmed infections.
Friday, WHO emergency response chief Peter Salama said many people vaccinated in Mbandaka received the shots more than 10 days ago, meaning they’re now protected – the vaccine has had time to kick in.
Finding people who need vaccination is much harder in the remote area of Iboko, where a new case was just reported. Shoddy infrastructure adds to the challenge. “The roads are so bad that even if a person gets vaccinated it can be too late and they can still die,” said Rosy Boyekwa Yamba, a regional representative for the Ministry of Health in Mbandaka.
It can take days to travel just 100 miles to reach remote areas where Ebola still is spreading. The vaccine must be kept at a temperature of minus 76 to minus 112 degrees Fahrenheit and can only be kept in mobile freezers for up to seven days.
DOES THE VACCINE WORK?
Health experts say the next two weeks will be critical in determining whether the outbreak will be brought under control. The organization has predicted there could be up to 300 cases of Ebola in the coming months.
No matter how the outbreak unfolds, U.S. CDC Ebola expert Dr. Pierre Rollin says, it will be nearly impossible to say whether the vaccine worked to stop the disease’s spread.
“We can say the vaccine plus all the other measures work, but you can’t say the vaccine by itself works,” he said. In order to do that a controlled test would have to be run where in one place only the vaccine is being used and in another it’s not being used at all.
Meanwhile, some recipients say the shot provided peace of mind. Mbandaka resident Marie Louise, 68, proudly slaps her vaccination papers on the table. “I get life with the vaccine,” she says.
Send questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.