YARMOUTH — I went to bed last night thinking about screaming. This morning, as I drove my son to work, I asked if he knew any good places to scream – places where I wouldn’t rouse the dogs or spook the chickens, and nobody would call 911. He said, “Try the woods by 295 and wait for a semi.”
Why would a mild-mannered elderly physician like me be looking for a place to scream?
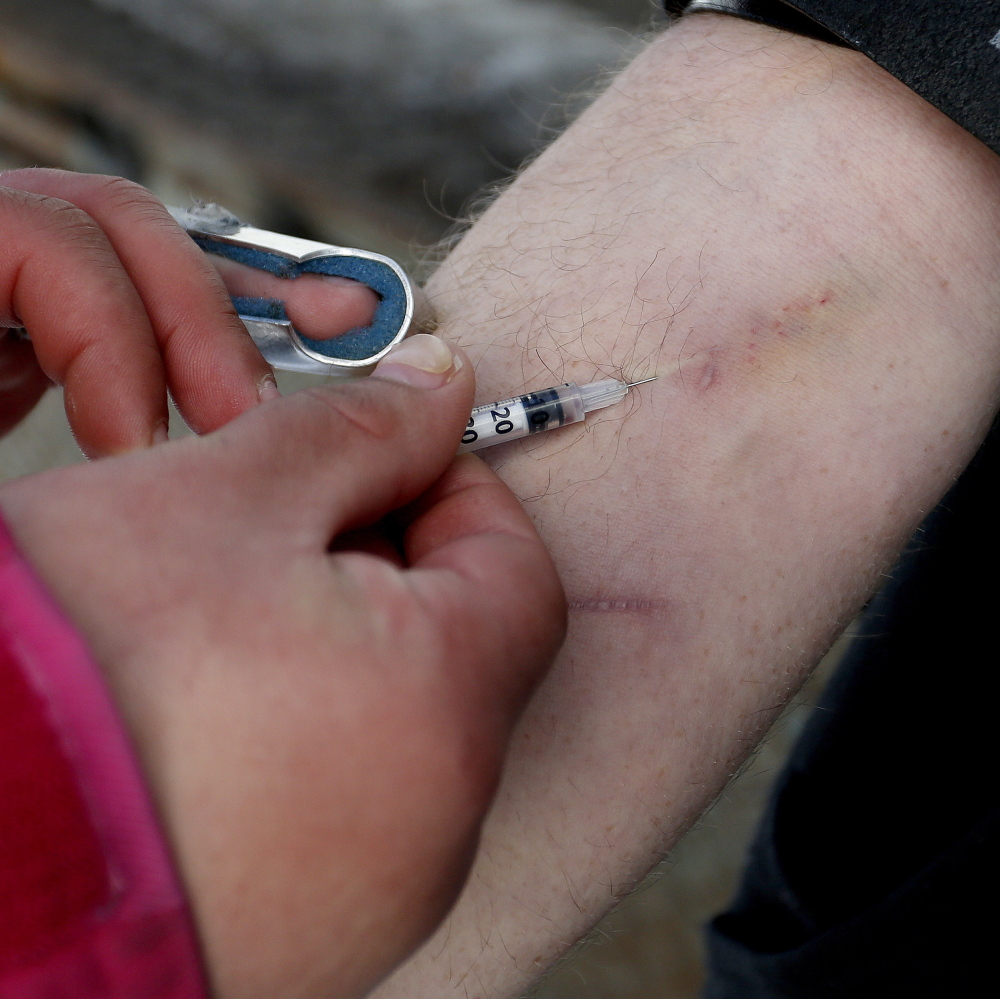
I treat heroin addicts. I see dozens every week. Since January 2014, when hundreds of them lost MaineCare, I have been able to do little for them beyond easing their withdrawal symptoms and sending them back out to the streets. Now I can’t even do that.
TREATMENT REQUIRES INSURANCE
The heroin they are using is cut with fentanyl, or sometimes is pure fentanyl, a more potent narcotic than heroin. Fentanyl has a high affinity for opiate receptors and stays in the system longer. Suboxone, the medicine I use to treat withdrawal, displaces more fentanyl from my patients’ opiate receptors and often makes them sicker.
So, even if I wait to treat them until they are in total misery with intractable vomiting and diarrhea, profound bone and joint pain, even if I wait until they are jumping out of their skin with restlessness and anxiety, they get worse – even though I think they can’t.
And I took an oath to do no harm.
My patients are young men and women – 18, 20, 22, 24 years old – from all over Maine. Some of them started partying in high school or middle school and found they couldn’t stop. Some got oxycodone for a twisted knee, or Vicodin when they got their wisdom teeth out, and that was all it took. Some come from generations of addiction and dysfunction.
Regardless of how they started, they are all desperate to stop. But they have no insurance. They cannot get treatment. They have no recourse but to come to detox over and over and over again, and try not to overdose when they leave.
So why can’t they just stop?
It’s a reasonable question. But addiction is a problem that reason, or judgment, or willpower can’t solve. Drugs hijack the most primitive part of our brain: the part that tells us what we need to do to survive. And opiates do it best.
Use for a month. You’ll get high at first. But soon, it’s not pleasure you’re seeking, it’s survival. You’re using to get you through the day. You’re shooting up just so you can function and not withdraw, just so you can feel normal.
You might ask: What about detox? Isn’t that enough is to get the drugs out of your system and change your life? The answer is “no.”
Craving for opiates is profound, trenchant and long-lasting.
Even after detox, even after months of recovery, even after years of sobriety, something will trigger a memory of use. The cravings will come back with a vengeance, and you’ll have a needle in your arm and wonder how it got there.
Why can’t my patients get treatment? Simple. Money.
There are some places in town where self-pay patients can go and get help. The cost is $300 to $500 for the first visit and $150 for all the following visits.
My patients don’t have that. Nor do they have the $600 a month that their Suboxone will cost, or the $360 a month for methadone.
A DESPERATE PROPOSAL
Hasn’t this crisis been in the headlines long enough? Haven’t enough of our children overdosed and died? How does denying my patients insurance or closing down Mercy Recovery Center make any sense?
Here’s a desperate proposal. I have room for 20 more Suboxone patients in my practice. Somebody give me a place to see them, a salary for a counselor, a medical assistant, money to fund lab work and meds, and I’ll see them for free.
My son says maybe I should get another job. But I love my patients and the work I do.
So roll down your windows on your way to work and maybe you’ll hear me out in the woods by the highway: a fierce, bitter howl of frustration at my inability to help these kids even at the most basic level, a long, keening wail of grief for a whole generation of Mainers whose lives are forfeit.
Copy the Story LinkSend questions/comments to the editors.


Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.