The parent company of Maine Medical Center has increased its investment in a sweeping new computer system that was designed to make it easier for patients and medical professionals to access health records but caused the company problems in its first year.
MaineHealth officials said most of the increase, from $145 million to $200 million, will be used to expand employees’ training, to fix problems related to learning the Epic software that led to millions of dollars in billing losses.
With the new system, Maine Medical Center failed to send out accurate bills, which became a major factor in the hospital’s loss of $13.4 million in the first six months of its 2013 fiscal year, officials have said.
Bill Caron, president of MaineHealth, said Epic had a rough start when it was installed at the state’s largest hospital in late 2012.
“It’s a good investment once you get it right,” he said, because the system makes it easier for patients to see their own records and for doctors and nurses to track what care has been provided. The system will be installed by 2017 throughout the MaineHealth system, which includes more than a dozen hospitals.
Caron said Epic will make the organization more efficient, reducing operating costs by eliminating the need for some back-office positions.
He said MaineHealth originally underestimated the resources needed to train employees to use Epic, and it might have been a mistake to start the new computer system with the 6,000-employee Maine Medical Center, MaineHealth’s largest employer.
“There were good arguments to be made on both sides,” Caron said, but in hindsight, it might have been better to start with a smaller, pilot project and then expand to larger parts of the MaineHealth network.
None of the startup problems was related to the software itself, said Andy Crowder, senior vice president and chief information officer for MaineHealth. “The program has performed as designed.”
Recognizing the training mistake, Caron said about two-thirds of the $55 million added in early December will go toward teaching the staff to use the program, while the remaining third reflects an increase in the scope of the program as MaineHealth has expanded.
In the three years since MaineHealth chose the Wisconsin-based Epic program, Memorial Hospital in New Hampshire and more private doctor practices have been added to the network.
Once Maine Medical Center started struggling with the implementation, startups were delayed at other MaineHealth hospitals, including Miles Memorial Hospital in Damariscotta, Pen Bay Medical Center in Rockport, St. Andrews Hospital in Boothbay Harbor and Waldo County General Hospital in Belfast.
For patients, the new system will make medical care better and less costly because there will be less duplication of services and fewer mistakes, said Dr. Jackie Cawley, chief medical officer for MaineHealth.
“The patient story is now following them, and the patients will be able to access their own records much easier,” Cawley said. Doctors and nurses will be able to see a patient’s medications, allergies, X-rays, and history of medical problems and other care.
The records will be updated in real time, so that a doctor’s note written in a hospital can be viewed by a primary care physician elsewhere 10 minutes later.
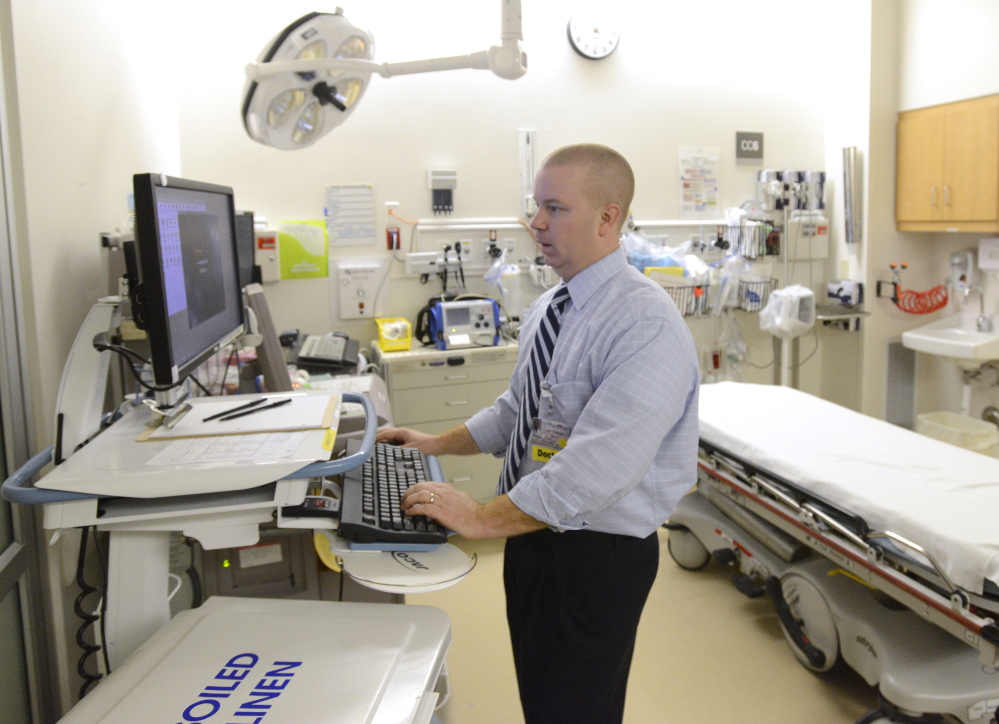
Dr. Nathan Mick said the system has made everything more efficient in Maine Medical Center’s emergency department, such as drastically reducing how much physicians have to write in longhand.
“In the (emergency department), it’s all about efficiency; it’s all about moving fast,” said Mick, who estimates the system has chopped an hour off the time it takes to admit a patient.
Mick said the software can be customized, so the department can constantly retool it to meet specific needs. The system will flag professionals when errors are about to be made.
“It will tell me if I’m about to be an idiot,” Mick said.
But Afton Trotter, an emergency room nurse, said that while Epic isn’t a problem by itself, the way it’s being used is making it more difficult at times for nurses to interact with patients, because the nurses have to spend so much time with computers.
“I’m not sure that the implementation of Epic at Maine Medical Center has had the same benefit to safe and patient focused care as it has had on increasing the ease of billing and increasing productivity,” Trotter said in a written statement. “In my practice safe medication administration is a lot more than bar code scanning and still requires a competent professional to think critically about the ârights’ of safe medication administration.”
In Falmouth, Dr. Rebecca Hemphill said she sees many benefits to the Epic system in her primary care practice.
“If my patient is in the hospital, I can see a doctor’s note that was written 10 minutes ago,” Hemphill said. “I can see lab results and everything that’s happening to them.”
Hemphill’s patient Bud Harris, 91, said he looks at his records all the time at home, and uses them to track his medications and write notes to his doctors.
“If I need to know anything, I just go to the computer,” Harris said.
Joe Lawlor can be contacted at 791-6376 or at:jlawlor@pressherald.comTwitter: @joelawlorph
Copy the Story LinkSend questions/comments to the editors.



Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.