Maine is undergoing its worst acute hepatitis C outbreak since it began recording cases in the 1990s. Reported cases of the disease have soared since 2013, corresponding with skyrocketing heroin use, and are more than triple the national average.
The heroin epidemic is causing many undesirable ripple effects in Maine, public health advocates say, including the spread of infectious diseases such as hepatitis C.
Hepatitis C is a blood-borne viral disease that attacks the liver, and is often spread by intravenous drug users sharing needles. It also can be contracted through unprotected sex or other contact with infected blood.
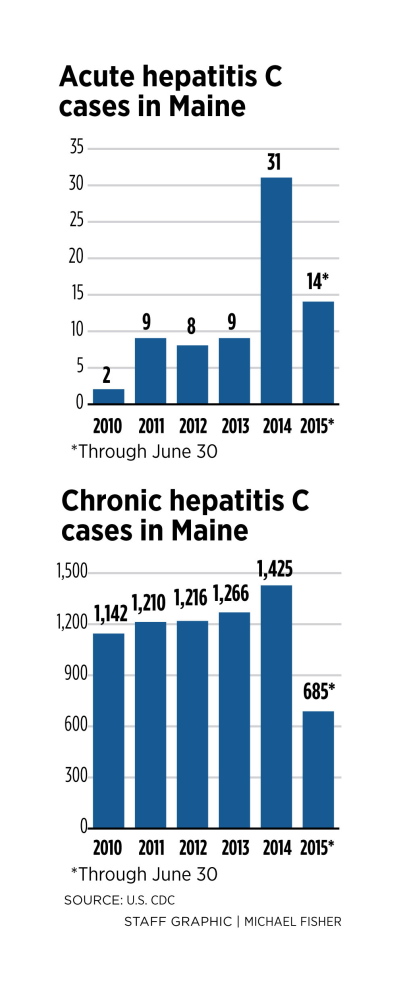
Acute cases – a six-month infection where symptoms manifest themselves – more than tripled from 2013 to 2014, from nine to 31, according to the Maine Center for Disease Control and Prevention.
At the same time, chronic hepatitis C – long-term infections that can sometimes last a lifetime – increased 25 percent, from 1,142 cases in 2010 to 1,425 in 2014.
Through June 30 this year, acute and chronic cases are tracking about the same as 2014, indicating that the outbreak is continuing, according to the state CDC.
Acute hepatitis C simply means that the infection is discovered within six months of contracting the disease. Most acute cases convert to chronic hepatitis C, but patients can have chronic hepatitis C that goes undetected for years.
The hepatitis C virus was discovered in 1989, and Maine began comprehensive reporting of cases in 1996.
Meanwhile, the number of those seeking treatment for heroin abuse more than tripled, from 1,115 in 2010 to 3,463 in 2014, according to the Maine Office of Substance Abuse.
TREATMENTS BETTER, BUT COSTLY
Treatments for hepatitis C have vastly improved over the past two years, with the introduction of new medications, but are expensive, according to the Food and Drug Administration.
The Maine CDC recognizes the hepatitis C problem and is developing a plan to better prevent and treat the disease, said John Martins, department spokesman.
“The increase in hepatitis C cases in Maine is most likely due to a combination of a true increase in the number of cases along with an increase in reporting,” Martins said in a prepared statement. He agreed that drug users sharing needles counts for part of the increase.
David Zysk, 33, of Wells, a former heroin user, said that although users are aware of hepatitis C and other diseases that can be transmitted by shared needles, such as HIV, staying safe is often not a priority when chasing the next drug high.
“I think it’s always in the back of your mind that this disease (hepatitis C) is out there,” Zysk said. “But the consequences of your decisions don’t always enter your mind, the addiction is that powerful.”
Zysk said he wasn’t always safe in how he handled needles for the 12 years he was a heroin addict.
“I’m lucky I don’t have it,” Zysk said of hepatitis C. He said there’s also a misconception among users that hepatitis C is not a difficult illness to manage.
NEEDLE EXCHANGE HELPS
At Portland’s needle exchange program operated by the city’s India Street Clinical Services, the staff has seen a surge in heroin users since 2013, during a time when treatment options are drying up. Self-identified heroin users have tripled from 1,400 in 2012 to 4,218 currently.
In 2014, 104 people using the Portland clinic tested positive for hepatitis C, about double the figure from 2012. Without the needle exchange program, hepatitis C cases would be even higher, said Dr. Caroline Teschke, clinic director.
“Ten cents for a needle, $90,000 for three months of hepatitis C treatments,” Teschke said. “There’s no comparison.”
Without a needle exchange program, about one-third of heroin users would contract the disease, but for those coming to the clinic for clean needles the rate is less than 20 percent, she said.
Teschke said keeping the current user population as safe as possible is only part of the solution. Maine is lacking in treatment options, especially for low-income addicts, and will soon have fewer resources when Mercy Recovery Center in Westbrook closes this summer.
“Treatment options are pitiably few and far between,” Teschke said.
Nationally, acute hepatitis C cases also have increased, although not as dramatically as in Maine, from 1,778 in 2012 to 2,138 in 2014.
Part of the reason is that New England has become a hotbed for heroin use, with national media reports noting a spike in heroin abuse in Vermont, New Hampshire, Maine and Massachusetts.
Teschke said users are switching from prescription opiates like OxyContin to heroin.
“Unfortunately, heroin is cheaper and it’s extremely available,” she said.
Teschke said she wishes needle exchange programs – which are currently in five locations around the state – were expanded to every county, along with improved access to treatment. She said government money is not available for the programs, which are often controversial because some say they promote drug use, and the programs operate on a shoestring budget.
STATE DEVELOPING STRATEGY
The state is studying the hepatitis C issue and developing strategies, Martins said in an email response to questions.
“The state strategy for reduction in hepatitis C cases is a combination of prevention, education, testing and linkage to care,” Martins said, noting a study that the Maine CDC is currently undertaking that surveys 18- to 24-year-olds who have been recently diagnosed with the disease.
Martins said the agency is promoting a “no-cost” hepatitis C screening that is available in many counties, and improved public education for patients and awareness among primary care doctors.
In the past two years, two new drugs, Sovaldi and Harvoni, have proven to be effective at treating hepatitis C, but the pills can cost $1,000 each, according to the FDA.
That often leaves the underinsured or uninsured out in the cold for the new treatments, Teschke said. She said about 60 percent of needle exchange users are uninsured.
Christine Purington, 59, of Augusta, who says she was cured of her hepatitis C, said she’s fortunate that her insurance covered the expensive treatments. Purington was diagnosed with the disease in 1999 – she doesn’t know how she contracted it and was not a heroin user – and underwent 15 years of treatments that left her tired and in pain.
“You just feel bad all the time,” Purington said. “I was always nauseous, always having joint pain, always fatigued.”
She began taking Sovaldi in September 2014, and by December her hepatitis C was cured, she said. Purington now feels much better, but she still finds it hard to believe she’s no longer afflicted. Purington said she wouldn’t wish the disease on anyone, and hopes the state figures out a way to combat it.
“As long as we have more addicts, it’s going to continue to increase,” she said.
Copy the Story Link
Send questions/comments to the editors.






Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.