WASHINGTON — The black mold creeping into the spines of hundreds of people who got tainted shots for back pain marks uncharted medical territory.
Never before has this particular fungus been found to cause meningitis. It’s incredibly hard to diagnose, and to kill — requiring at least three months of a treatment that can cause hallucinations. There’s no good way to predict survival, or when it’s safe to stop treating, or exactly how to monitor those who fear the fungus may be festering silently in their bodies.
“I don’t think there is a precedent for this kind of thing,” said Dr. Arjun Srinivasan of the Centers for Disease Control and Prevention. Health officials and doctors have tracked down most of the 14,000 people potentially at risk for fungal meningitis, blamed for the deaths of 24 people and sickening more than 300.
“This is definitely new territory for us,” he said.
The fungus’ brown-black color signals an armor that — along with being injected near the spine —helped this mold sneak past the immune defenses of otherwise healthy people, said Dr. Arturo Casadevall, a fungal disease specialist at New York’s Albert Einstein College of Medicine.
“What we’re dealing with here is fundamentally different” from a typical fungal infection, he said. “This is a bug that most of us don’t know much about.”
But they’re learning fast, piecing together clues that promise some hope.
Doctors are beginning to detail in medical journals the first deaths in this outbreak, and the grim autopsy findings make clear that treating early is crucial, before the fungus becomes entrenched. In one case, a woman died in Maryland after the fungus pierced blood vessels in her brain, leading to severe damage.
People getting treated earlier “seem to be doing OK,” with fewer of the strokes that characterized the outbreak’s beginning, said Dr. Carol Kauffman of the University of Michigan. She has advised the CDC and co-authored advice in the New England Journal of Medicine on how to handle the complex medication used in treatment.
People who got contaminated steroid shots made by a Massachusetts pharmacy have been told to be on guard for months for meningitis symptoms. But the CDC said Wednesday that the biggest risk for getting sick seems to be within 42 days of receiving one of the implicated back injections.
With the tainted shots recalled in late September, that means the period of greatest risk is nearing an end. And it should help doctors bombarded with calls from the worried determine who most needs a spinal tap to look for the very earliest signs of infection.
The CDC said doctors have two valid options: To watch patients closely for symptoms or to consider a just-in-case spinal tap, possibly repeated weekly, for at-risk people still inside that 42-day window. However, CDC officials note that spinal taps come with their own risks.
“We know the farther out you are from receiving an injection, the lower your risk becomes for developing meningitis or other infections. We want to emphasize that,” CDC’s Dr. Tom Chiller told a conference call for physicians on Thursday.
Still, public health officials recall a 2002 meningitis cluster linked to steroid injections contaminated with a different fungus; one of those victims got sick 152 days after the shot.
Fungal infections don’t get a lot of attention, but they afflict millions around the world, said David Perlin of the University of Medicine and Dentistry of New Jersey, who is studying better ways to diagnose them. Most are skin infections like athlete’s foot, but fungi also can cause pneumonia, sinusitis and other problems.
Serious infections tend to strike people with immune systems weakened because of cancer, AIDS or other problems. Fungus-caused meningitis in particular is extremely rare— especially in otherwise healthy people like in this outbreak — and it’s “very bad news,” said Michigan’s Kauffman.
While the more common bacterial and viral forms of meningitis tend to strike quickly with obvious symptoms, fungal meningitis grows very slowly and is hard to diagnose. Few antifungal drugs are absorbed into the central nervous system, limiting treatment options. Plus, human cells and fungal cells have a lot of similarities, making it hard to attack the fungus without side effects, Kauffman explained.
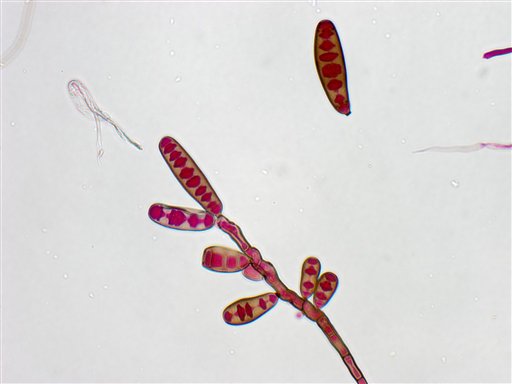
The main culprit in this outbreak is a black mold called Exserohilum rostratum, common in dirt and grasses. Only 33 human infections previously had been reported, mostly eye or skin infections in people with weak immune systems, Casadevall said.
Here’s how scientists think it’s sneaking into the well-guarded spinal cord and brain of a healthy person:
—The steroid injected near the spine reduces inflammation, one of the immune system’s defenses against contamination.
—The mold grows quietly until enough accumulates for it to burrow a tiny hole, or abscess, into the lining of the spinal canal, said Dr. William Schaffner of Vanderbilt University. Reaching the spinal fluid inside offers a direct pathway to the brain.
—The fungus’ color signals how intractable it is. Brown-black molds produce melanin, the same chemical that helps human skin tan. It guards against the sun’s mold-killing ultraviolet rays — and inside people, it fends off both antifungal drugs and other immune-system attacks, Casadevall said.
The good news: Black mold is treatable with a drug named voriconazole, with far fewer side effects than the older treatment initially recommended when the outbreak began.
Still, Kauffman cautioned doctors to carefully monitor patients because differences in metabolism can make levels surge in the bloodstream, causing hallucinations, confusion, nausea and occasionally liver damage. On the flip side, their bodies may process the drug too quickly to battle the fungus. Plus, voriconazole can interact badly with a list of other common medications.
“It’s not clear” how long to treat but at least three months is advised, Kauffman said. It begins with intravenous infusions that are hard to administer outside of a hospital. Then once the patient is stable enough, pills can be used.
Copy the Story Link
Send questions/comments to the editors.


Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.