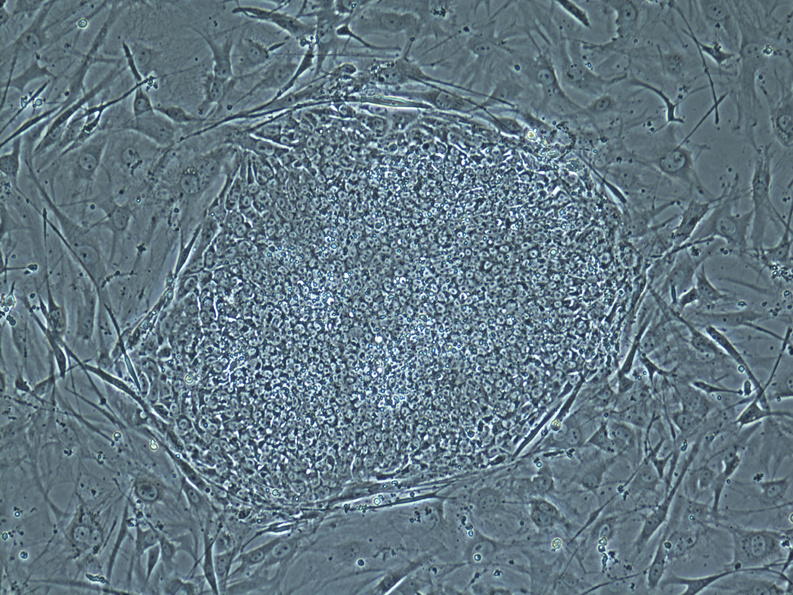
NEW YORK — Scientists have finally recovered stem cells from cloned human embryos, a longstanding goal that could lead to new treatments for such illnesses as Parkinson’s disease and diabetes.
A prominent expert called the work a landmark, but noted that a different, simpler technique now under development may prove more useful.
Stem cells can turn into any cell of the body, so scientists are interested in using them to create tissue for treating disease. Transplanting brain tissue might treat Parkinson’s disorder, for example, and pancreatic tissue might be used for diabetes.
But transplants run the risk of rejection, so more than a decade ago, researchers proposed a way around that: Create tissue from stem cells that bear the patient’s own DNA, obtained with a process called therapeutic cloning.
If DNA from a patient is put into a human egg, which is then grown into an early embryo, the stem cells from that embryo would provide a virtual genetic match. So in theory, tissues created from them would not be rejected by the patient.
That idea was met with some ethical objections because harvesting the stem cells involved destroying human embryos.
Scientists have tried to get stem cells from cloned human embryos for about a decade, but they’ve failed. Generally, that’s because the embryos stopped developing before producing the cells. In 2004, a South Korean scientist claimed to have gotten stem cells from cloned human embryos, but that turned out to be a fraud.
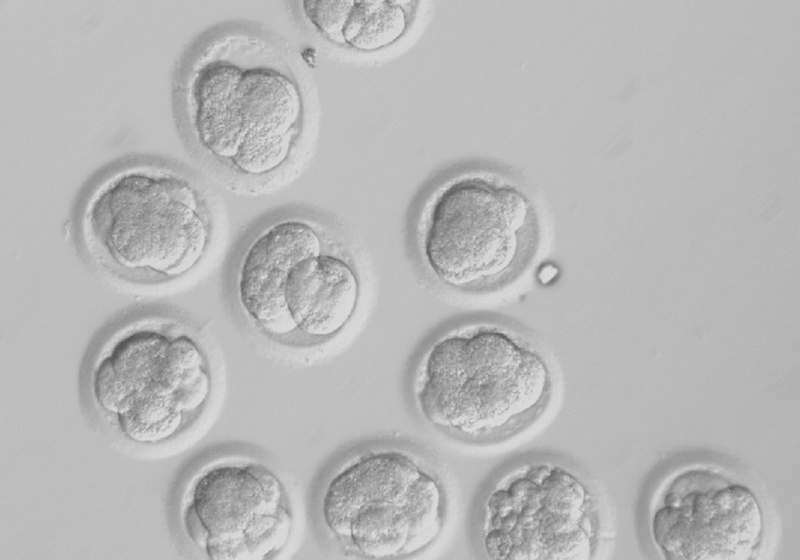
In Wednesday’s edition of the journal Cell, however, scientists in Oregon report harvesting stem cells from six embryos created from donated eggs. Two embryos had been given DNA from skin cells of a child with a genetic disorder, and the others had DNA from fetal skin cells.
Shoukhrat Mitalipov of the Oregon Health & Science University, who led the research, said the success came not from a single technical innovation, but from revising a series of steps in the process. He noted it had taken six years to reach the goal after pursuing it with monkey embryos.
Mitalipov also said that based on monkey work, he believes human embryos made with the technique could not develop into cloned babies, and he has no interest in trying to do that. Scientists have cloned more than a dozen kinds of mammals, starting with Dolly the sheep.
The new work was financed by the university and the Leducq Foundation in Paris.
Dr. George Daley, a stem cell expert at Boston Children’s Hospital who didn’t participate in the work, called the new results “one landmark step in a very long journey” toward creating DNA-matched transplant tissue.
Now, Daley said, scientists must compare the embryo-cloning approach with another technology that reprograms blood or skin cells directly into substitutes for embryonic stem cells. This reprogramming approach, reported in 2007, is technically simpler and doesn’t involve embryos or require the donation of human eggs.
But these substitute cells show some molecular differences compared to embryonic ones, which has led to questions about whether they can safely be used for treating patients. So it’s essential to compare the cells from the two methods, Daley said.
Send questions/comments to the editors.


Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.