Linda Dennison’s early detection scan at Mercy Hospital came back negative for lung cancer, despite her history as a pack-a-day smoker who picked up the habit at age 13.
“I am embarrassed that I still smoke,” said Dennison, whose brother died of lung cancer a few weeks ago. She had her 45-second scan last week, followed by enrollment in a smoking cessation program. “I’m very determined to quit,” she said.
Dennison, 64, of Baldwin, was one of hundreds of smokers – soon to be thousands – who have received CT scans for lung cancer at the Portland hospital.
Mercy and other hospitals are combining the scans with smoking cessation programs to both detect lung cancer early enough to treat it more effectively and to provide smokers with visual evidence of the damage that cigarettes cause, which might convince them to quit.
Driving the push to increase use of the scans is Medicare’s decision in February to allow them as a covered benefit for longtime smokers age 55 or older. Previously it was an out-of-pocket cost, with typical charges of $200 to $400. Mercy charges $250 out-of-pocket.
Most insurance companies are expected to follow Medicare’s lead and start including the scans as a covered benefit, Mercy doctors said.
“Even if you’re paying for it out-of-pocket, if you think about what you’re spending on cigarettes, it’s a good deal,” said Dr. Chris Kuhn, a Mercy radiologist.
The program is expanding at Mercy and at several other hospitals around the state, including Maine Medical Center and Central Maine Medical Center, according to an official with the Maine chapter of the American Lung Association. Both Maine Med and Mercy started limited CT scans for lung cancer in 2013. At Mercy, officials plan to promote the scans and further pair the procedure with smoking cessation efforts.
Because the program is new, the hospitals haven’t kept track of how many times the CT scans have been used for lung cancer screening.
LEADING CAUSE OF CANCER DEATHS IN U.S.
Lung cancer is deadly if not caught early. A patient diagnosed with late-stage lung cancer has only a 5 percent chance of living five more years, compared with about 50 percent if the cancer is caught earlier, according to the International Association for the Study of Lung Cancer.
“It’s very effective for the group it was designed for,” said Ed Miller, an American Lung Association spokesman. He said he hopes the scans will soon be standard at most Maine hospitals.
“There are not many symptoms for early stage lung cancer, but if you catch it early, you can do something about it,” Miller said.
Lung cancer is the leading cause of cancer deaths in the United States, according to the American Lung Association. Maine – the oldest state – has a higher rate of lung cancer deaths – 52 per 100,000 population in 2011, the latest year for which data is available – than the national average of 46 deaths, according to the U.S. Centers for Disease Control and Prevention.
That translates to about 1,000 deaths per year in Maine, and 150,000 nationally. Maine’s adult smoking rate, at 19 percent in 2014, has plummeted since the 1990s, but is similar to the national average, according to Partnership for a Tobacco-Free Maine.
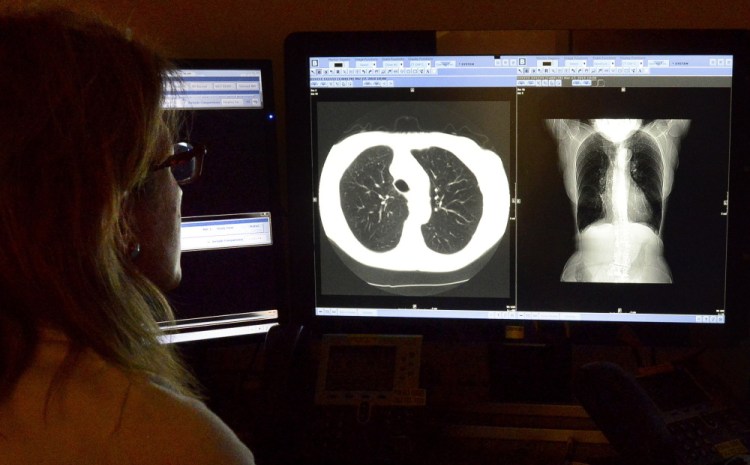
While CT scans that provide 3-D imaging of internal organs have been available for many years, the imaging software has improved to the point that the scans can be done with much lower radiation doses while still providing a good image, doctors said. The scans can detect tumors when they are relatively tiny, when treatment is likely to be more effective. Chest X-rays are notoriously ineffective at detecting lung cancer, doctors said.
EARLY DETECTION CAN MAKE A DIFFERENCE
Mercy officials said that because the patient sees the results of the scan during the same appointment, longtime smokers confront their lifetime of unhealthy choices during a “moment of truth.” They can also see through the imaging how much their smoking has damaged their lungs, even if the scan comes back negative for cancer.
Dr. Elena Wechsler, a Mercy radiologist, said the drama of the appointment, including waiting for the scan, is a motivator for patients.
“Certainly, we see a lot of teary-eyed patients. But we sit with them, and we can use that moment to encourage them that they need to stop smoking. Being with them is comforting to them,” Wechsler said. “Many of the patients have wanted to quit, but have been putting off quitting for a very long time.”
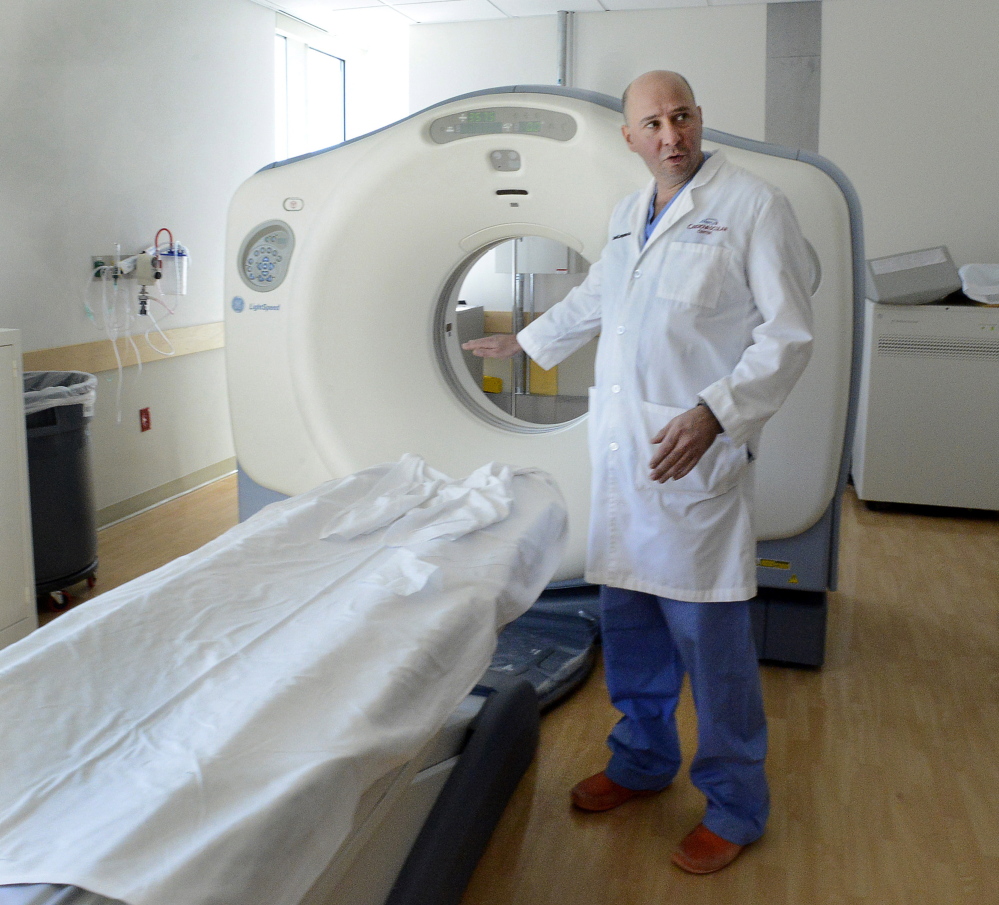
Kuhn said most hospitals already have the CT scan equipment, which will make it easier to expand such programs.
Research has shown that scans, and resulting early detection, can decrease lung cancer deaths by 20 percent, which led Medicare to adopt the scan as a covered benefit.
“That’s a ‘wow’ result, and we do not get a lot of those in medicine,” Kuhn said.
Dr. Paul Han, director of the Center for Outcomes Research and Evaluation at the Maine Medical Center Research Institute, agreed that CT scans for lung cancer should be expanded, but carefully. Han noted that 25 percent of the tests produce false positives, which can cause unnecessary anxiety and increase costs for the patient, hospital and insurance company.
“It’s still kind of a blunt instrument. It’s good enough and yet inaccurate enough that it poses a dilemma,” Han said.
He said the best uses for the scans are those in the “highest of the high-risk” patients, and that maybe, over time, hospitals can develop methods to accurately identify that population so they don’t unnecessarily test people who don’t have symptoms.
Han said another issue is that even though radiation from a CT scan is low, it’s still subjecting the patient to radiation. Patients should not have too many scans, or the scans themselves could cause cancer.
“It’s kind of an unknown,” Han said. “We think the risk is small, but we don’t really know.”
Still, Han said the scans have a “modest benefit,” and Maine Med plans to expand the program and pair it with a “robust” smoking cessation program.
Han said another factor is that as technology keeps improving, the images will be even better than they are now. That should lead to the scans becoming more accurate at detecting lung cancer, leading to fewer false positives.
‘NO DOUBT I WAS GOING TO DO THIS’
The price of treating late-stage lung cancer, which most often still results in death, is also a factor, Kuhn said. It costs an average of $48,000, compared with $33,000 for two years of lung cancer treatment discovered in earlier stages, according to an October 2014 report in the Journal of Thoracic Oncology. And if the program results in more long-term smokers quitting, that will also save money and lives, Kuhn said.
Dennison said she has long wanted to quit, but the death of her brother, a heavy smoker, motivated her to finally sign up for the scan.
She said she adopted two pre-teen children, and she wants to be alive when they become adults.
“I am the only one in the family who smokes,” Dennison said. “If I don’t quit, there’s a good chance I’m not going to be here. When my brother died, there was no doubt I was going to do this.”
Dennison said she takes the drug Chantix, which curbs nicotine cravings, and talks frequently with an anti-smoking “coach” at Mercy. She also deposits coins into a “money jar” to represent how much money she is saving by not buying cigarettes.
In about a week on the program, Dennison has cut her habit from one pack a day to half a pack.
“The scan came out clean, so I thought, ‘Let’s keep it that way,’ ” Dennison said.
Dennison, who doesn’t smoke inside the house, says she’s had enough of smoking in rainstorms and snowstorms.
“This has given me a sense of self-confidence that I can do this,” she said. “It’s time to step up to the plate and quit smoking.”
Copy the Story Link
Send questions/comments to the editors.




Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.