If you are an expectant mom and planning to breast-feed, Maine is a great place to have your baby.
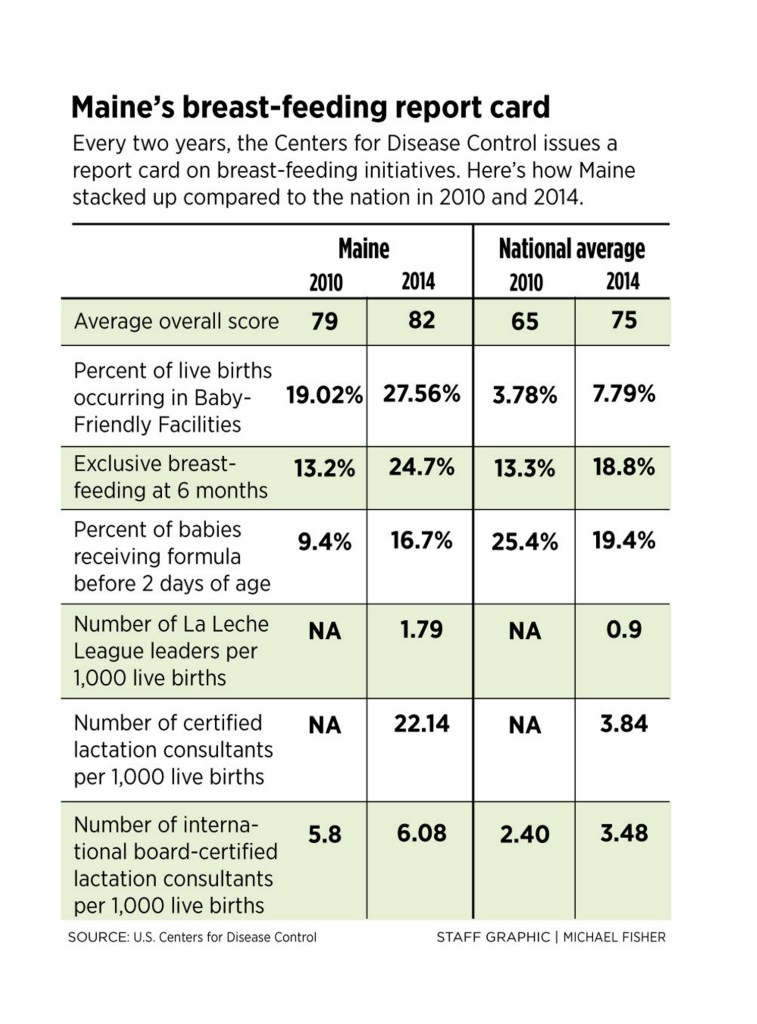
Maine scores higher than the national average on the U.S. Centers for Disease Control’s Breastfeeding Report Card, which assesses support metrics and success rates in each state. It also has a higher-than-average rate of hospitals that have been certified as “Baby Friendly,” a designation that reflects multiple practices to foster successful breast-feeding.
This means that they have implemented the 10 best practices outlined by the World Health Organization and UNICEF to foster successful breast-feeding. Nearly 30 percent of Maine’s birthing facilities are certified as Baby Friendly, surpassing the national average of 7 percent. In Maine, nearly one-third of all births occur at a baby-friendly hospital, compared to just 7.2 percent nationwide.
Maine likely has such an outstanding record on breast-feeding because of its active coalitions, said Dora Anne Mills, vice president for clinical affairs for the University of New England and former director of the Maine CDC.
“They’ve done an excellent job of bringing together a variety of partners and women’s health care providers,” Mills said, noting the state’s small size and collaborative nature have helped boost local breast-feeding initiatives and success rates.
“We have a small number of hospitals and health care providers, and they tend to work very collaboratively compared to other states, that are not just bigger geographically, but also have bigger populations,” she said. “It’s such an interconnected culture here, and we’re like one big small town rather than a state. So when a couple of hospitals adopt policies on something like breast-feeding, and they see what has worked, other hospitals readily follow.”
THE BENEFITS OF BREAST-FEEDING
The WHO and American Academy of Pediatrics recommend that moms exclusively breast-feed for at least six months, and continue to supplement solid foods with breast milk for up to two years.
Research has shown that cells, hormones and antibodies in breast milk help lower babies’ risks of asthma, leukemia, obesity, ear infections, eczema, lower respiratory infections, SIDS and Type 2 diabetes.
Moms benefit, too. A review of studies published in the November 2015 issue of Annals of Oncology showed that breast-feeding protects against certain types of breast cancers. A study in the December 2015 issue of Annals of Internal Medicine concluded that among women who developed gestational diabetes, those who breast-fed more frequently, and for longer, were less likely to develop Type 2 diabetes after delivery.
In 1991, WHO and UNICEF launched the Baby-Friendly Hospital Initiative, and created Baby Friendly USA to certify hospitals that have adopted its top 10 best practices. In Maine, six of the 27 birth hospitals have received the certification, including Bridgton Hospital, Central Maine Medical Center, LincolnHealth, Maine General Medical Center, Stephens Memorial Hospital and York Hospital.
LincolnHealth earned the baby-friendly certification in 1997, the fifth hospital in the nation and the first hospital in Maine to do so. In the past, up to half of the moms who delivered at LincolnHealth came from outside the region. But as other hospitals have focused on promoting breast-feeding, those numbers have dropped, said Lynn Plumb, nurse manager of obstetrics for LincolnHealth.
“It’s really what you want – to have women have many choices of where to go to have a wonderful birth experience,” Plumb said. “You really want everyone to be striving to support breast-feeding, and support formula feeding when the mother has issues (like medication or surgery) which make breast-feeding impossible.”
She pointed out that many of WHO’s 10 best practices – like rooming in and skin-to-skin contact – also support moms who choose to formula feed.
“There are a lot of things about becoming ‘baby friendly’ that support the whole community of women having babies,” said Plumb.
Twenty-three years after WHO and UNICEF set their best practices, the Maine CDC, Maine State Breastfeeding Coalition and MaineHealth developed “6 for ME” to improve breast-feeding success rates, said Debra Wigand, director of Maine’s Division of Disease Prevention. The program identified six of the top 10 as the most important practices, and created training and support to help local health care professionals adopt them.
GOING BEYOND
Those practices include establishing and communicating an evidence-based breast-feeding policy, educating new parents about the benefits of breast-feeding and establishing support for it after discharge.
Maine Medical Center, for instance, has increased education requirements for staff and boosted the number of lactation consultants on staff from five to eight, said Kara Kaikini, lactation and childbirth education program manager for the hospital’s Family Birth Center.
For new and expectant moms, the hospital holds weekly breast-feeding support groups and classes.
The hospital has also developed initiatives to increase rooming-in rates, and reduced the number of times when babies are given formula as supplemental nutrition in the early days of life, said Kaikini.
Maine Med is exploring expanding the use of pasteurized donor human milk into its Mother Baby Care unit for babies who may need more than their mother’s milk to help raise blood sugar levels. This option has been available for certain premature or ill babies in the hospital’s neonatal intensive care unit.
At Southern Maine Health Care in Biddeford, one particularly successful practice has been encouraging skin-to-skin contact between moms and newborns within 60 to 90 minutes of delivery, said Lindsay Toppen, a registered nurse and lactation consultant who heads up the hospital’s breast-feeding task force.
Skin-to-skin contact has been associated with higher breast-feeding success rates and delivers a host of other health benefits to newborns.
“These babies are much more stable,” said Toppen. “Moms have these incredible (breast) milk supplies coming in sooner than before, and babies’ weights are plateauing and coming up sooner. We’ve seen huge jumps in our success rates.”
Some of the goals have been more challenging to implement.
Rooming in encourages moms to room with their babies for 23 out of the 24 hours a day. Studies show that moms get just as much sleep when their babies room in as they do when babies are in the nursery.
It also gives staff an opportunity to educate new parents about safe sleep and breast-feeding habits, she added.
But it can be a tough sell to both new parents and staff, said Toppen. Staff are accustomed to taking babies to the hospital nurseries at the request of exhausted parents. Now they are being encouraged to offer assistance and support for rooming in.
At Maine Med, “if mom is physically and emotionally exhausted after a difficult labor and birth and asks for some rest time without baby in her room, we honor her wishes,” Kaikini said. “We then make sure we bring baby back to her as soon as she (or baby) requests it.”
Educating parents about what to expect in the days after delivery is also critical to successful breast-feeding.
At Southern Maine Health Care, moms are encouraged to have advocates with them in the hospital – especially if the other parent has to be home with older children – and to develop a plan for how they will manage rest and recovery after they deliver.
Just like they have a birthing plan, “the postpartum period is just as important to plan for,” Toppen said.
Copy the Story LinkSend questions/comments to the editors.




Success. Please wait for the page to reload. If the page does not reload within 5 seconds, please refresh the page.
Enter your email and password to access comments.
Hi, to comment on stories you must . This profile is in addition to your subscription and website login.
Already have a commenting profile? .
Invalid username/password.
Please check your email to confirm and complete your registration.
Only subscribers are eligible to post comments. Please subscribe or login first for digital access. Here’s why.
Use the form below to reset your password. When you've submitted your account email, we will send an email with a reset code.