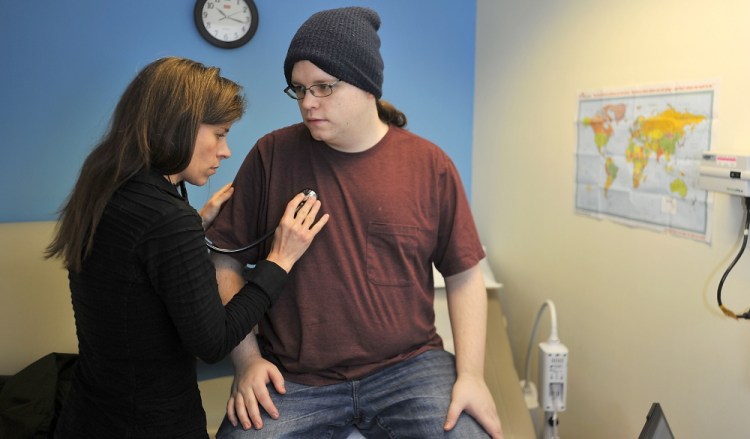
At the Portland Community Health Center, patients pack into a small waiting room to see harried doctors and nurses for primary care services such as vaccines, checkups and to acquire antibiotics for infections.
Increasingly, the patients do not have MaineCare – the state’s name for Medicaid – and are instead uninsured, leaving the health center facing a financial crunch that if not addressed would threaten the clinic’s existence.
That’s because the dollars-and-cents difference for the clinic between seeing a MaineCare patient or an uninsured patient is dramatic.
From uninsured patients, who pay on a sliding scale based on their income, the clinics would typically receive about $10 or $20 per visit. But if the patient has MaineCare, the state would reimburse the clinic about $150 to $200, depending on what services are provided. MaineCare is a state-run health insurance program for low-income residents funded with a blend of federal and state dollars.
Since Maine trimmed eligibility for MaineCare, reducing the ranks of Medicaid patients from 357,000 in 2011 to about 290,000 this year, community health centers have increasingly felt the financial fallout.
The Portland health center has seen its revenue drop by $1 million – out of a $4.1 million budget – and without financial help it would have to close or refuse to accept all new patients. The center is on track to be unable to pay its bills at the end of the fiscal year in June, when it’s projected to have a $500,000 deficit with no cash reserves.
“With this patient mix, our business model does not work,” said Leslie Clark, the center’s CEO. “Ideally, we would have a reserve. We don’t have any reserves. We can’t cut staff anymore.”
A RELIANCE ON MAINECARE
The clinic relies on MaineCare income for more than half of its operating budget, but it has seen its MaineCare reimbursements plummet from $2.9 million in 2010 to $1.9 million this year. The clinic is also funded directly by the federal government and other grants.
Portland is not the only community health center feeling the pinch. Centers in Sanford, Eastport and elsewhere are reporting financial problems, according to an executive who represents the clinics.
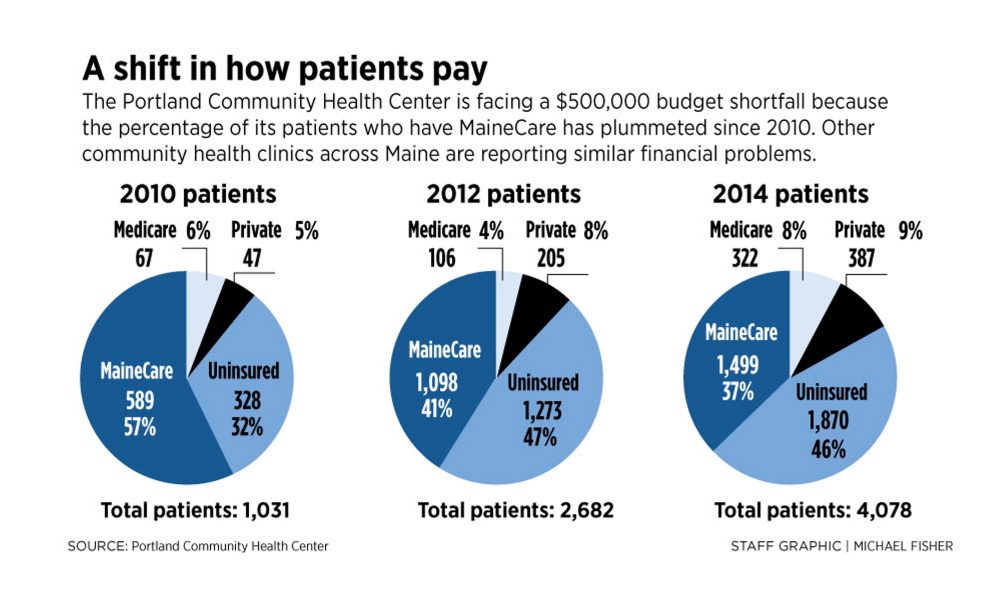
Four years ago, before Gov. Paul LePage’s administration began reducing the MaineCare rolls, Medicaid patients made up 57 percent of all patients at the Portland center. That number has gone down as fewer people are eligible for MaineCare, and it was reduced even further during the latest MaineCare cutback in January 2014, when the state tightened eligibility requirements, removing 25,000 childless adults and parents from the rolls.
Now, only 37 percent of the center’s patients are on Maine-Care, and 46 percent are uninsured, compared to a 32 percent uninsured rate in 2010. Meanwhile, most of the people who have gained insurance coverage through the Affordable Care Act go elsewhere for treatment, Clark said. Maine’s overall uninsured rate has declined from 16.1 percent in 2013 to 13.3 percent in 2014, but more of the uninsured in the Portland area appear to be going to the Portland clinic.
The center serves 4,000 patients, triple its 2010 patient population. The problem, Clark said, is that about half of all new patients are uninsured.
By law, community health clinics are not permitted to refuse new uninsured patients while still accepting MaineCare patients. The clinics must treat everyone who walks in the door, but can refuse to see all new patients. But at the Portland clinic, refusing to see all new patients does not fit with its mission, and it does not help the situation because the current mix of patients is financially unsustainable, Clark said.
Clark said that after LePage was re-elected governor in November – effectively ending any chance for Medicaid expansion – the center was left looking at budget cuts to stay afloat. It cut $300,000 and left a few vacancies unfilled, but now, with an ever-growing patient population, the center can’t cut anymore, she said, and still be able to deliver services.
“Our whole goal was to get through the year and get MaineCare expanded,” Clark said.
Dr. Renee Fay-LeBlanc, chief medical officer at the Portland health center, said she ran in a fundraiser in Florida and collected several thousand dollars in donations for patients who can’t afford their prescriptions, such as antibiotics.
“It’s really challenging on a day-to-day basis right now. We’re under so much financial stress,” Fay-LeBlanc said.
ASKING ADMINISTRATION FOR HELP
The problem is so acute that the Maine Primary Care Association, which represents the state’s 17 health clinics, is asking the LePage administration to pump $3 million into the clinics over two years.
“This is an untenable situation. At some point there comes a breaking point,” said Vanessa Santarelli, CEO of the primary care association. “Our need is much greater than what we’re asking.”
Santarelli said she has met with the administration but has not received any signals that it would support the funding, although she said the clinics have pledges of support from Democrats and Republicans in the Legislature.
Although it’s not clear whether the administration will support the request, LePage’s proposed two-year state budget would devote more money to primary care reimbursements, providing more than $15 million a year to offset federal cutbacks. David Sorensen, Maine Department of Health and Human Services spokesman, said the agency had no comment on the issue because it has not yet received a formal funding request from the clinics.
Santarelli said she hopes the LePage administration’s emphasis on primary care funding will bode well for the $3 million budget request.
In Eastport, Holly Gartmayer-DeYoung, CEO of the Eastport Health Care clinic, said the reduced MaineCare reimbursements are having a “devastating effect,” and she worries about being able to finish the year in the black. Gartmayer-DeYoung said she didn’t yet have a backup plan for when the money runs out.
“I don’t know what we’re going to do. It’s a nightmare. I have sleepless nights worrying about it,” she said.
FEWER SERVICES FOR UNINSURED
Martin Sabol, executive director of Nasson Health Care in Sanford, said the situation there is “not as dire” as in Portland, which serves a much higher uninsured population, but it, too, is feeling financial strains from having more uninsured patients.
Newly uninsured patients who were previously on MaineCare also receive fewer services, and have to rely entirely on clinic services instead of at times being referred to other doctors who take MaineCare patients.
For Joss Beane, 33, of Portland, losing his MaineCare coverage in January 2014 sent him into a “deep depression.”
“I was in a bad state of depression for nine months,” said Beane, who suffers from post-traumatic stress disorder and depression. “I’m finally getting to the point where I feel like I can start contributing again.”
Still, Beane said he notices that the Portland health center cannot provide the same level of services as when he was on MaineCare. For instance, when he had MaineCare coverage, he could go to the health center and then be referred to a psychiatrist for counseling. Now, he is briefly counseled by a social worker at the clinic, which does not offer extensive, in-house mental health services.
Beane said he also needs a tooth pulled, which can’t be done at the health center, but would have been covered by MaineCare. He said he’s going to somehow scrounge up money to get his aching tooth removed. Beane said he gets angry about the many people who are in the same situation as he is – no longer having MaineCare coverage.
“If something serious happened to me, it would be really crushing, financial and otherwise,” Beane said. “Accidents happen, and people get all kinds of injuries and maladies.
“We’re still out here. We’re not just going to disappear.”
Send questions/comments to the editors.



Comments are no longer available on this story